Anthony Coetzer-Liversage*,†, Pete Nelson*, Ben Suker*
ABSTRACT
Recovery Corps is a pioneering social innovation in behavioural health, addressing the critical need for peer-driven recovery support services amidst the ongoing substance use crisis in the United States. Leveraging AmeriCorps infrastructure, Recovery Corps recruits and trains individuals with substance use disorder (SUD) lived experience to provide peer support in underserved communities. This narrative examines central assumptions associated with the Recovery Corps initiative, including those related to a perceived unmet demand for peer support, the feasibility of training community members without professional backgrounds, the impact of Recovery Corps peer support on recovery outcomes, and the degree to which Recovery Corps experience creates career pathways for individuals in recovery. By bridging service gaps, enhancing recovery capital, and fostering sustainable workforce development, Recovery Corps offers a comprehensive model for integrating peer support within behavioural health frameworks. Lessons drawn from Recovery Corps underscore the importance of capacity building, flexible evaluation methods, and strategic partnerships to sustain and scale peer-driven interventions. This program highlights an adaptable approach to recovery support, presenting a model that may inform future social innovation in behavioural health.
Key Words Recovery; peer support; career pathway; substance use; implementation; scale.
The escalating substance use crisis in the United States has created an urgent need for innovative approaches to recovery support. In 2023, approximately 48.5 million adults reported having a substance use disorder (SUD), highlighting demand for scalable, cost-effective solutions to address the complex needs of individuals with SUDs (Substance Abuse and Mental Health Services Administration (SAMHSA), 2023a, 2023b). This trend underscores the necessity for strategies that improve engagement, enhance recovery outcomes, and bolster intervention efficacy. Many researchers focus on developing evidence-based interventions (EBIs) but often neglect studying their implementation (Weisz et al., 2014). As a result, EBIs, though well researched, lack the necessary implementation strategies for real-world effectiveness, leaving practitioners to rely more on personal experience than data to guide efforts (Albers et al., 2020).
Peer-based recovery support services, leveraging lived experiences, have shown promise in improving recovery outcomes, including treatment adherence, relapse prevention, and building supportive networks (Bassuk et al., 2016; du Plessis et al., 2019; Tracy & Wallace, 2016). Recovery capital, encompassing the social, physical, human, and cultural resources needed for sustained recovery (Cloud & Granfield, 2008; Hennessy, 2017), is central to these services. Peer support interventions enhance recovery capital by addressing personal and systemic challenges faced by individuals in recovery (Drazdowski et al., 2024; Eddie et al., 2019). However, most organizations lack the capacity to deliver these services at scale and the data infrastructure to assess their implementation and impact. Existing research also overlooks the perspectives of practitioners and policymakers crucial for effective implementation (Powell et al., 2012, 2015).
This social innovation narrative highlights Recovery Corps (RC), an initiative designed to expand peer support services and improve understanding of peer support implementation and impact by creating a rich data infrastructure for evaluation. Using the AmeriCorps infrastructure, RC recruits, trains, and places Peer Navigators in diverse settings, adhering to the SAMHSA standards (SAMHSA, 2023a, 2023b). By integrating linkage facilitation (Hogue et al., 2024) and personalized recovery navigation (Griswold et al., 2010; Stowell et al., 2022), it aims to improve recovery outcomes and address the gap in peer support research. Additionally, RC embeds evaluation within practice, aligning with Albers et al.’s (2020) call for continuous feedback loops to ensure the model’s effectiveness.
RC stands out by reversing the traditional model of evidence-based practice, using data-informed outreach to refine its peer support services. This approach aligns with Albers et al.’s (2020) emphasis on integrating implementation science with real-world practice, ensuring that empirical evidence guides the development of recovery strategies. By generating practice-based evidence, the program contributes to broader implementation science, while addressing both immediate recovery needs and systemic change (Coetzer-Liversage et al., 2024). It exemplifies a scalable intervention model, capable of expanding from small settings to real-world conditions while maintaining effectiveness (Milat et al., 2013).
The RC model also addresses a gap in implementation science by engaging practitioners, policy leaders, and other stakeholders in the development of peer support interventions (Weisz et al., 2014). This collaboration ensures that implementation strategies are evidence based and tailored to the specific needs of those implementing the interventions. RC reflects Albers et al.’s (2020) call for partnerships between researchers, practitioners, and policymakers to enhance successful implementation.
In the following sections, we explore RC as a social innovation, examining its implementation, effectiveness, and impact on recovery capital, offering insights for scaling peer-based models in broader substance use intervention frameworks.
RC development began in 2017, driven by the need to bolster the capacity of organizations serving individuals in recovery in Minnesota. A planning grant from AmeriCorps enabled a community-engaged and team-based approach of collaboration with state recovery leaders, researchers, and practitioners, leading to a recovery boot camp hosted by Hazelden Betty Ford in 2016. In addition, Minnesota’s state AmeriCorps service commission (ServeMinnesota) created an Opioid Response Task Force, composed of 15 Minnesota leaders and recovery experts. This task force, including a state senator and two members of the Minnesota House of Representatives, played a key role in informing the initiative’s efforts, convening quarterly as thought partners to support the state’s response to opioid-related substance use broadly and the launch of RC specifically.
Public engagement was also a central component of the initial development strategy, exemplified by participation in events such as The Opioid Crisis: The Response from Minnesota in October 2018. This event attracted recovery professionals, legislators, a pharmaceutical representative, AmeriCorps members, and state service commissioners. The forum featured speakers such as Peter Gaumond from the Office of National Drug Control Policy, Liz Farmer, fiscal reporter for Governing magazine, and Leslie Crutchfield, author of How Change Happens: Why Some Social Movements Succeed While Others Don’t, while also prioritizing the voices of individuals with opioid use disorder lived experience to ensure a grassroots perspective was provided (Cheng & Smith, 2009). Finally, RC benefited from consultative support from Dr. John Kelly, Director of Harvard’s Recovery Research Institute, and an AmeriCorps-funded partnership with community engagement researchers at the University of Virginia in 2019. This collaboration aimed to further understand the needs of the population served, with particular focus on underserved groups.
RC was developed in accordance with peer support standards established by SAMHSA (2023a, 2023b). By integrating the principles outlined by Albers et al. (2020), RC addresses critical gaps in recovery services through strategic partnerships with local networks that pave the way for RC members – referred to as “Navigators” – to provide peer support. Navigators are trained in motivational interviewing (Miller & Rollnick, 2023), linkage facilitation (Hogue et al., 2024), and goal setting. Leveraging their lived experience, Navigators cultivate trust, enhance self-efficacy, and promote long-term recovery while addressing participants’ social, personal, and community recovery needs (Čtvrtečková et al., 2024).
Navigators are placed in a variety of settings to provide individualized peer support, including recovery community organizations, health services organizations, collegiate recovery organizations, harm reduction organizations, non-profit health care services, treatment centres, recovery residences, and state and local agencies (e.g., Department of Corrections). They are supervised to ensure compliance with AmeriCorps rules, track progress, and conduct evaluations. In addition, an RC program manager provides Navigator oversight, maintains site relationships, and supports Navigator development. To foster community engagement and reflection, monthly Corps Days provide members with opportunities to connect with one another and the community, consistent with recommendations for ongoing professional development and community integration found in the literature (Albers et al., 2020).
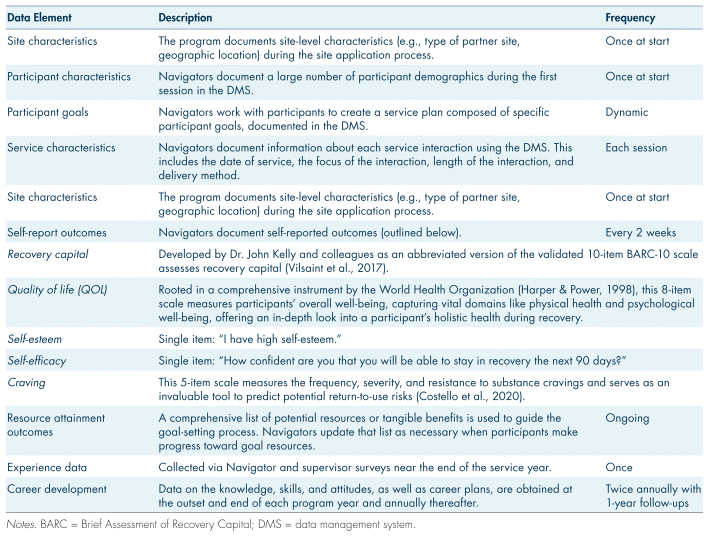
Navigators regularly integrate data into their service using an internally developed data management system (DMS) to inform services. In addition to DMS-sourced data, RC collects experience data from Navigators and supervisors annually and assesses the professional and personal development of Navigators using a career development survey at multiple time points within and across years of program participation. The data infrastructure for RC enables continuous feedback loops to assess program implementation and its overall efficacy. An overview of the RC data elements is provided in Table I.
TABLE I Data elements for Recovery Corps
As an emerging innovation in the peer support environment, there are a number of important assumptions to consider: (1) that there is significant need for additional peer support services at organizations across the nation, (2) that untrained community members with SUD lived experience can be trained to deliver peer support services with adequate dosage and fidelity, (3) that the support provided produces meaningful impacts on those served, and (4) that RC creates meaningful post-service career pathways for people in recovery who are interested in peer support. In this section, we draw from DMS data and survey data to focus explicitly on indicators of implementation – including dosage and scale over time – as well as indicators of efficacy to illustrate potential for this community-driven model as an avenue for increasing service provision, creating pathways for long-term peer support careers, and advancing research- to-practice linkages.
Through diverse partnerships, RC provides critical capacity for peer support and also collaborates with site partners to learn and adapt the model to meet local needs. This approach to partnership builds trust, enhances recovery outcomes across regions, and is consistent with the collaborative approach recommended by Albers et al. (2020) for effective implementation. Since its inception in Minnesota, the RC program has expanded to Illinois and Virginia, with significant growth in both Navigators and individuals served (Table II). For example, the number of partnering sites increased substantially from 16 in Minnesota (2020–2021) to 76 across multiple states (2023–2024). Navigator numbers also rose, with Minnesota growing from 43 to 94 Navigators, Illinois from 17 to 38, and Virginia from 37 to 95. That growth highlights the potential of an AmeriCorps-driven infrastructure for scaling promising interventions and provides evidence of a deep capacity gap to provide peer support services. Relatedly, survey data from site supervisors lend additional evidence for the match between the program and site needs. For example, supervisors (N = 55) across all three states indicated agreement that the program had a positive impact on their site (98%), had a positive impact on site beneficiaries (98%), fit within the culture and values of the site (96%), and provided resources or services that would otherwise not be provided (91%). Further, 95% of supervisors indicated that Navigator training and coaching prepare them to enter the peer support workforce.
TABLE II Implementation measures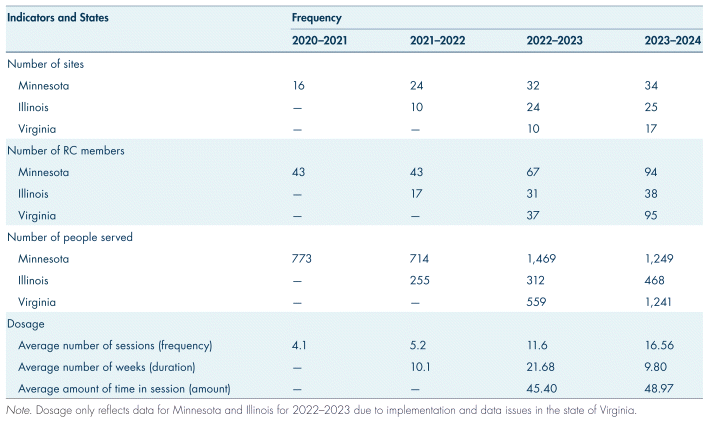
Intervention dosage data – including duration (time spent receiving support), frequency (number of interactions), and amount (session length) – provide a critical reference for understanding assumptions about capability of Navigators to deliver peer support in practice, as well as how continuous feedback loops and program monitoring might be used to strengthen dosage across time (Metz & Bartley, 2020).
In the case of RC, the average number of interactions between Navigators and participants increased from 4.10 in 2020–2021 to 16.56 in 2023–2024, indicating improved engagement. The average duration and length of support have remained relatively consistent over time, with most Navigators providing support for approximately 10 weeks, and each interaction lasting about 45 minutes. These trends may provide insight on typical dosage in practice and highlight RC’s commitment to optimizing peer support dosage, which is linked to improved outcomes (Ashford et al., 2021). Few applied studies report on dosage and optimization of participant engagement to improve outcomes (Vayshenker et al., 2016), providing RC an opportunity to expand the literature in this area as it reports on dosage and participant outcomes tracking.
As outlined previously, RC also captures information about the format of peer support delivery as it has important influences on implementation fidelity (Malaguti et al., 2020). Unlike elements of intervention dosage, characteristics related to the format of service delivery were relatively stable across time, with 64% of interactions delivered in person, 34% by phone, and 2% by video sessions in 2023–2024. Individual sessions were by far the most dominant format (85%), with group sessions making up 15%, reflecting the program’s adaptability to meet participant and contextual needs (Table III).
Existing research provides promising evidence for the impact of peer support (Ashford et al., 2021; Reif et al., 2014); however, leveraging AmeriCorps as an entry point for delivering peer support across a diverse population of sites types is somewhat different in nature, making insight on the degree to which the application of peer support in this context produces positive benefits.
When examining pre-post scores on a variety of health outcomes measures collected by RC, there is evidence of meaningful growth each year, with average gains tending to increase in concert with program scaling and continuous improvement efforts. More specifically, scores for recovery capital, quality of life, and self-efficacy showed significant gains, alongside increased substance-free days (Table IV). Recovery capital in particular saw substantial improvements, with a paired samples t-test t-score of 11.72 and a p value of 0.000 by the end of 2023–2024 (Table V). These gains are generally consistent with those observed in published correlational research conducted under similar conditions (Ashford et al., 2021). For example, Ashford et al. reported a 1.33-point increase in recovery capital among 3,459 people who received peer support at recovery community organizations for an average of 18.7 weeks and 9.75 sessions, whereas RC has observed larger gains in the last 4 years.
TABLE V Pre- and post-analysis of recovery capital
Additionally, RC Navigators also reported on the impact of their work on community participants through the Member Experience Survey. This survey captured Navigators’ (N = 110) perceptions of their influence, with 99% indicating a positive impact on those they served throughout the year.
As we note above, RC is designed to introduce additional pathways into a peer support career or related career in the recovery field. To evaluate the viability of that design, the program collects data on the knowledge, skills, career interests, and employment of Navigators at the outset and conclusion of service. In general, those data indicate that the program significantly impacts Navigators by improving their skills and career prospects. For example, examining data from 2023–2024, notable advancements were observed across all career capital scores – “Knowing Why,” “Knowing What,” and “Knowing Who” – as detailed in Table VI, with all improvements showing statistical significance (p = 0.000). By the end of the service year, 28% of recovery Navigators had secured employment, and 38% were seeking employment. Additionally, 54% of members chose to return for another year of service. Many also indicated plans to pursue further education, including certifications, associate degrees, and bachelor’s degrees, enhancing their professional development. This supports existing literature which highlights that professional growth and self-efficacy are key outcomes for peers involved in recovery support roles (du Plessis et al., 2019).
TABLE VI Recovery Corps Navigator career capital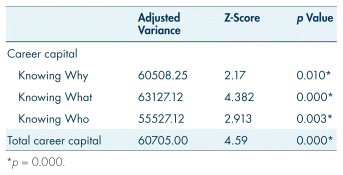
A thematic analysis (Braun & Clarke, 2012) of Navigators’ experiences (2023–2024) identified several key themes (Table VII), emphasizing professional growth, challenges, and impact of their work. The major themes were Personal Growth and Self-Care, Support and Advocacy, Professional Development, Community Impact and Empowerment, and Challenges and Reflections. The experiences of Navigators highlight the importance of managing personal well-being while fulfilling their roles, with a focus on setting boundaries and prioritizing self-care to prevent burnout. Their advocacy work, navigating complex systems, and providing emotional support were central to helping individuals overcome barriers and achieve their goals. Professional development was a critical part of their journey, with continuous learning and adaptation essential for enhancing their effectiveness. Moreover, their work made a significant impact on the community, empowering individuals and families. Lastly, Navigators’ reflections on overcoming challenges demonstrated their resilience and professional growth. These themes provide further consistent findings with the existing literature which show the personal and professional benefits that providing peer support services has on the peer (du Plessis et al., 2019).
TABLE VII Thematic analysis of RC Navigators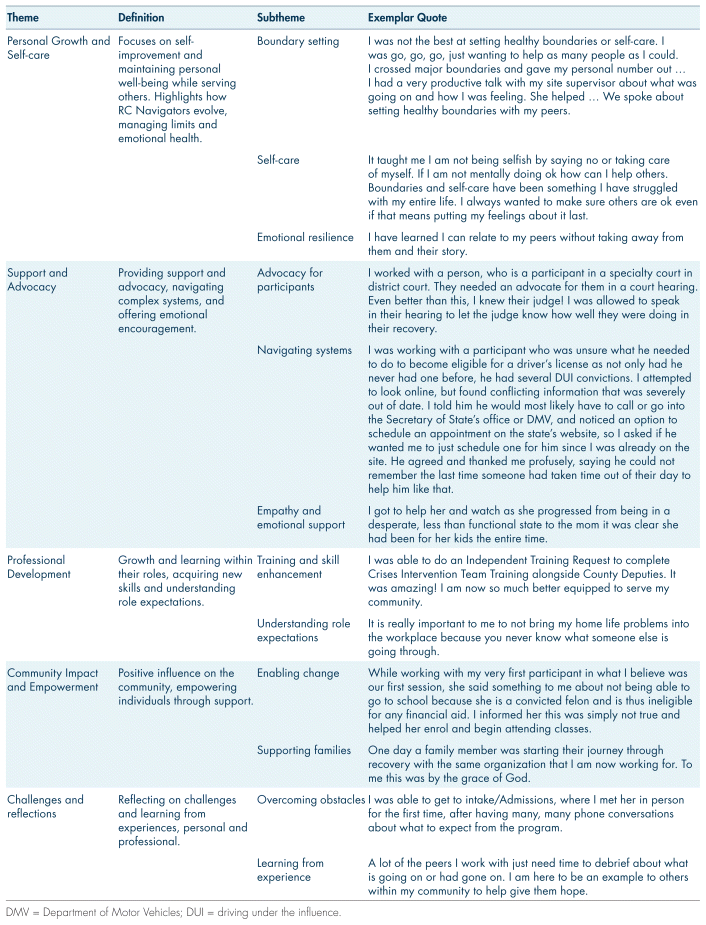
Preliminary evaluation data for the RC program illustrate its potential as a transformative entry point for peer support careers, offering a feasible and impactful model that introduces a diverse workforce to the recovery field. This initiative brings new individuals into the peer support profession, demonstrates positive career and skill-building outcomes for its members, and produces meaningful benefits for the people served by its members. However, an examination of RC also illustrates potential challenges – some specific to RC and others reflective of those faced more broadly within peer support. For example, scaling the program and generating rigorous evidence on its impact require significant resources, planning, and partnership. Due to the dynamic, relational nature of peer support, designing and implementing experimental evaluations can be complex. Addressing these challenges requires strengthening internal research capacity, fostering external partnerships, and engaging site partners who are committed to evidence-based practices.
The diversity of implementation contexts within RC also provides valuable insights into how different settings influence outcomes. This variance allows the program to assess how factors like site partner onboarding and peer integration impact the effectiveness of peer support, yet it also introduces variability that can hinder consistency. That is, the manner in which different organizations believe “peer support” should be operationalized differs, and those beliefs influence implementation. Challenges in site placement and peer integration, such as inadequate job descriptions and limited site staff understanding, align with existing literature on peer workforce integration barriers (Albers et al., 2020; Bauer et al., 2015). To address these issues, RC has implemented structured coaching for site partners to support effective onboarding and enhance implementation fidelity, consistent with evidence-based recommendations for sustainable program impact (Fleddermann et al., 2023). However, as peer support becomes increasingly prevalent in a variety of contexts, the impact of site environments on the delivery of peer support is an area in need of future research.
RC provides valuable lessons for advancing peer support models in behavioural health, built on four key assumptions that inform the feasibility and scalability of the program and broader peer support strategies.
These lessons illustrate RC’s role as a pioneering model in behavioural health, establishing that peer-driven support is both feasible and impactful in underserved areas. By addressing service gaps, fostering workforce development, and validating the recovery impact of peer support, RC lays a foundation for advancing peer support as a core component of sustainable recovery initiatives.
Building on these lessons, RC demonstrates the powerful role of peer support models in behavioural health, offering a framework that addresses service gaps, trains individuals in recovery to deliver effective support, and opens career pathways for them. The program’s success emphasizes the value of building internal capacity, forming research partnerships, and developing the behavioural health workforce. Lessons from RC highlight the need for adaptable implementation and evaluation methods to fully capture peer support’s impact, guiding future programs in scaling and sustaining these models for lasting recovery benefits.
We appreciate the valuable involvement of all those mentioned in this narrative along with all those who were not but had a large impact on the development, evaluation, and sustenance of Recovery Corps. Most importantly, we thank those with SUD lived experience who are the cornerstone of this program.
Recovery Corps is funded by AmeriCorps (22ACEMN001 and 24ACEMN001).
The authors declare that they are the employees of ServeMinnesota, the state commission responsible for Recovery Corps design and evaluation.
No ethics board approval was needed, as all data are part of program implementation and evaluation; however, all participants provided informed consent that the data collected as part of the implementation of the program can be used for research and publication purposes. Importantly, all precautions were taken to protect the participant information and confidentiality.
*ServeMinnesota, Minneapolis, MN, USA;
†Department of Psychology, University of Rhode Island, Kingston, RI, USA
Albers, B., Shlonsky, A., Mildon, R. (Eds.). (2020). Implementation science 3.0. Springer.
Crossref
Ashford, R. D., Brown, A., Canode, B., Sledd, A., Potter, J. S., Bergman, B. G. (2021). Peer-based recovery support services delivered at recovery community organizations: Predictors of improvements in individual recovery capital. Addictive Behaviors, 119, 106945. https://doi.org/10.1016/j.addbeh.2021.106945
Crossref PubMed
Bassuk, E. L., Hanson, J., Greene, R. N., Richard, M., Laudet, A. (2016). Peer-delivered recovery support services for addictions in the United States: A systematic review. Journal of Substance Abuse Treatment, 63, 1–9. https://doi.org/10.1016/j.jsat.2016.01.003
Crossref PubMed
Bauer, M. S., Damschroder, L., Hagedorn, H., Smith, J., Kilbourne, A. M. (2015). An introduction to implementation science for the non-specialist. BMC Psychology, 3, 1–12. https://doi.org/10.1186/s40359-015-0089-9
Crossref
Braun, V., Clarke, V. (2012). Thematic analysis. American Psychological Association.
Cheng, R., Smith, C. (2009). Engaging people with lived experience for better health outcomes: Collaboration with mental health and addiction service users in research, policy, and treatment. Ontario Ministry of Health and Long-Term Care.
Cloud, W., Granfield, R. (2008). Conceptualizing recovery capital: Expansion of a theoretical construct. Substance Use Misuse, 43(12–13), 1971–1986. https://doi.org/10.1080/10826080802289762
Crossref PubMed
Coetzer-Liversage, A. P., Stein, L. A. R., Stephens, M., Jefferis, E., Step, M., Crowe, A. R., Sloboda, Z. (2024). A human-centered innovation process (HCIP) for evidence-based substance use prevention intervention implementation. Health Behavior Research, 7(3). https://doi.org/10.4148/2572-1836.1265
Crossref
Costello, M. J., Viel, C., Li, Y., Oshri, A., MacKillop, J. (2020). Psychometric validation of an adaptation of the Penn Alcohol Craving Scale to assess aggregated drug craving. Journal of Substance Abuse Treatment, 119, 108127. https://doi.org/10.1016/j.jsat.2020.108127
Crossref PubMed
Čtvrtečková, M., Stromšíková, A., Roman, L. (2024). Role of peer support in building motivation to change addictive behaviour. The British Journal of Social Work, 54(2), 687–703. https://doi.org/10.1093/bjsw/bcad236
Crossref
Drazdowski, T. K., de Martell, S. C., Sheidow, A. J., Chapman, J. E., McCart, M. R. (2024). Leveraging parents and peer recovery supports to increase recovery capital in emerging adults with polysubstance use: Protocol for a feasibility, acceptability, and appropriateness study of launch. JMIR Research Protocols, 13(1), e60671. https://doi.org/10.2196/60671
Crossref PubMed PMC
du Plessis, C., Whitaker, L., Hurley, J. (2019). Peer support workers in substance abuse treatment services: A systematic review of the literature. Journal of Substance Use, 25(3), 225–230. https://doi.org/10.1080/14659891.2019.1677794
Crossref
Eddie, D., Hoffman, L., Vilsaint, C., Abry, A., Bergman, B., Hoeppner, B., Weinstein, C. Kelly, J. F. (2019). Lived experience in new models of care for substance use disorder: A systematic review of peer recovery support services and recovery coaching. Frontiers in Psychology, 10, 1052. https://doi.org/10.3389/fpsyg.2019.01052
Crossref PubMed PMC
Fleddermann, K., Jacobson, N., Horst, J., Madden, L. M., Haram, E., Molfenter, T. (2023). Opening the “black box” of organizational coaching for implementation. BMC Health Services Research, 23(1), 106. https://doi.org/10.1186/s12913-022-08948-6
Crossref
Griswold, K. S., Pastore, P. A., Homish, G. G., Henke, A. (2010). Access to primary care: Are mental health peers effective in helping patients after a psychiatric emergency? Primary Psychiatry, 17(6), 42–45.
Harper, A., Power, M. (1998). Development of the World Health Organization WHOQOL-BREF quality of life assessment. Psychological Medicine, 28, 551–558. https://doi.org/10.1017/S0033291798006667
Crossref
Hennessy, E. A. (2017). Recovery capital: A systematic review of the literature. Addiction Research Theory, 25(5), 349–360. https://doi.org/10.1080/16066359.2017.1297990
Crossref
Hogue, A., Satcher, M. F., Drazdowski, T. K., Hagaman, A., Hibbard, P. F., Sheidow, A. J., Coetzer-Liversage, A. P., Mitchell, S. G., Watson, D. P., Wilson, K. J., Muench, F., Fishman, M., Wenzel, K., de Martell, S. C., Stein, L. A. R. (2024) Linkage facilitation services for opioid use disorder: Taxonomy of facilitation practitioners, goals, and activities. Journal of Substance Abuse and Treatment, 157, 209217. https://doi.org/10.1016/j.josat.2023.209217
Malaguti, A., Ciocanel, O., Sani, F., Dillon, J. F., Eriksen, A., Power, K. (2020). Effectiveness of the use of implementation intentions on reduction of substance use: A meta-analysis. Drug and Alcohol Dependence, 214, 108120. https://doi.org/10.1016/j.drugalcdep.2020.108120
Crossref PubMed
Metz, A., Bartley, L. (2020). Implementation teams: A stakeholder view of leading and sustaining change. In: B. Albers, A. Shlonsky, R. Mildon (Eds.), Implementation science 3.0 (pp. 199–225). Springer. https://doi.org/10.1007/978-3-030-03874-8_8
Crossref
Milat, A. J., King, L., Bauman, A. E., Redman, S. (2013). The concept of scalability: Increasing the scale and potential adoption of health promotion interventions into policy and practice. Health Promotion International, 28(3), 285–298. https://doi.org/10.1093/heapro/dar097
Crossref
Miller, W. R., Rollnick, S. (2023). Motivational interviewing: Helping people change and grow (4th ed.). The Guilford Press.
Powell, B. J., McMillen, J. C., Proctor, E. K., Carpenter, C. R., Griffey, R. T., Bunger, A. C., Glass, J. E., Yok, J. L. (2012). A compilation of strategies for implementing clinical innovations in health and mental health. Medical Care Research and Review, 69(2), 123–157. https://doi.org/10.1177/1077558711430690
Crossref
Powell, B. J., Waltz, T. J., Chinman, M. J., Damschroder, L. J., Smith, J. L., Matthieu, M. M., Proctor, E., Kirchner, J. E. (2015). A refined compilation of implementation strategies: Results from the Expert Recommendations for Implementing Change (ERIC) project. Implementation Science, 10(1), 21. https://doi.org/10.1186/s13012-015-0209-1
Crossref PubMed PMC
Reif, S., Braude, L., Lyman, D. R., Dougherty, R. H., Daniels, A. S., Ghose, S. S., Salim, O., Delphin-Rittmon, M. E. (2014). Peer recovery support for individuals with substance use disorders: Assessing the evidence. Psychiatric Services, 65(7), 853–861. https://doi.org/10.1176/appi.ps.201400047
Crossref PubMed
Stowell, M. A., Thomas-Gale, T., Jones, H. E., Binswanger, I., Rinehart, D. J. (2022). Perspectives among women receiving medications for opioid use disorder: Implications for development of a peer navigation intervention to improve access to family planning services. Substance Abuse, 43(1), 722–732. https://doi.org/10.1080/08897077.2021.2007514
Crossref PubMed PMC
Substance Abuse and Mental Health Services Administration (SAMHSA). (2023a). Low barrier models of care for substance use disorders (Advisory: Publication No. PEP23-02-00005). SAMHSA Administration. https://library.samhsa.gov/sites/default/files/advisory-low-barrier-models-of-care-pep23-02-00-005.pdf
Substance Abuse and Mental Health Services Administration (SAMHSA). (2023b). Incorporating peer support into substance use disorder treatment services. Treatment Improvement Protocol (TIP) Series, No. 64. Publication No. PEP23-02-01-001. Substance Abuse and Mental Health Services Administration. https://www.ncbi.nlm.nih.gov/books/NBK596262/
Tracy, K., Wallace, S. P. (2016). Benefits of peer support groups in the treatment of addiction. Substance Abuse and Rehabilitation, 7, 143–154. https://doi.org/10.2147/SAR.S81535
Crossref PubMed PMC
Vayshenker, B., Mulay, A. L., Gonzales, L., West, M. L., Brown, I., Yanos, P. T. (2016). Participation in peer support services and outcomes related to recovery. Psychiatric Rehabilitation Journal, 39(3), 274. https://doi.org/10.1037/prj0000178
Crossref PubMed
Vilsaint, C. L., Kelly, J. F., Bergman, B. G., Groshkova, T., Best, D., White, W. (2017). Development and validation of a Brief Assessment of Recovery Capital (BARC-10) for alcohol and drug use disorder. Drug and Alcohol Dependence, 177, 71–76. https://doi.org/10.1016/j.drugalcdep.2017.03.022
Crossref PubMed
Weisz, J. R., Ng, M. Y., Bearman, S. K. (2014). Odd couple? Reenvisioning the relation between science and practice in the dissemination-implementation era. Clinical Psychological Science, 2(1), 58–74. https://doi.org/10.1177/2167702613501307
Crossref
Correspondence to: Anthony Coetzer-Liversage, ServeMinnesota, 120 South 6th St #2260, Minneapolis, MN 55402, USA. Telephone: 612-333-7740. E-mail: anthony@serveminnesota.org
This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/. For commercial re-use, please contact sales@sgpublishing.ca.
Journal of CSWB, VOLUME 10, NUMBER 2, June 2025