Marine Tessier*,†, Christine Genest†,‡
ABSTRACT
Public safety personnel (PSP), including police officers and firefighters, face significant risks of psychological issues due to exposure to traumatic events at work. Nevertheless, obstacles hinder seeking support. Understanding barriers and facilitators is crucial for tailoring interventions, to narrow the gap between need and action in seeking professional mental health support. The aim of this study is to provide a qualitative analysis of perceptions regarding seeking professional mental health support after being exposed to traumatic events at work in these two groups of PSP and identify potential differences between them. Based on 62 participants’ interviews (30 police officers and 32 firefighters), our findings informed us about current barriers to seek professional support as well as potential facilitators in police and firefighters’ organizations in the Quebec province of Canada. Six main themes were identified as barriers to seeking professional support among these PSP: opposing professional culture, accessibility issues, peer judgment, internalized stigma, prioritization of other coping strategies, and lack of self-awareness. Four main themes were identified that could facilitate the call for professional mental health support: organizational commitment, tailored resources, specific training, and peer-normalized attitudes. Some differences were found between the two occupational groups. Identifying barriers and proposing solutions assist organizations in supporting their employees’ mental health, while acknowledging potential differences between occupational groups that underscores the need for tailored support strategies.
Key Words Public safety; mental health services; occupational stress; barriers to care; traumatic events; police; firefighters.
Public safety personnel (PSP) are defined as frontline personnel in charge of population safety (Government of Canada, 2016). In the course of their duties, PSP are routinely exposed to emergency situations with a high potential for psychological trauma. As a result, they constitute an occupational group at elevated risk for mental health challenges, including depression, anxiety, post-traumatic stress disorder (PTSD), and suicidal ideation. Police officers and firefighters are primary representatives of the wider PSP population. According to research among Canadian municipal/provincial police officers, 19.5% presented symptoms of PTSD, 19.6% symptoms of depression, 14.6% symptoms of generalized anxiety, and 11.9% mentioned having suicidal behaviours in the past year (Carleton et al., 2018a, 2018b). As for Canadian firefighters, 13.5% presented symptoms of PTSD, 20.2% symptoms of depression, 11.7% symptoms of generalized anxiety, and 11.5% presented suicidal behaviours in the past year (Carleton et al., 2018a, 2018b).
Various risk and protective factors can influence the general psychological distress experienced by police officers and firefighters. According to previous studies, individual risk factors included chronic stress associated with the work context (Quarshie et al., 2021; Syed et al., 2020) and exposure to potentially traumatic events (Carleton et al., 2018c; Chopko et al., 2014). Job satisfaction/meaning, family support, or positive coping skills have been identified as protective individual factors for the mental health of PSP (Edgelow et al., 2023). Organizational risk factors included atypical work schedule (Boivin & Boudreault, 2022) and barriers to help-seeking (Geoffrion et al., 2023; Haugen et al., 2017). Regarding protective organizational factors, a strong sense of organizational belonging and supportive relationships with managers and peers have been linked to better mental health outcomes among employees (Chu et al., 2016; Encrenaz et al., 2016).
Obstacles to help-seeking primarily refer to the stigma surrounding psychological distress and barriers to accessing mental health services. The literature addressing these risk factors highlights several contributing elements, including a lack of awareness regarding available resources, concerns about confidentiality, fear of judgment within the organizational context, the belief that services are ill-equipped to understand the specific challenges faced by PSP, and structural barriers within the system (Bernier, 2021; Geoffrion et al., 2023; Haugen et al., 2017; Johnson et al., 2020; Jones et al., 2020). There are also factors that facilitate help-seeking, including the recognition that others are experiencing similar challenges, the perception that the issue has become overwhelming, previous positive encounters with mental health professionals, or the encouragement of peers (Jones et al., 2020). The literature addressing these barriers and facilitators often treats PSP as a homogenous group, without differentiating between specific sectors. PSP share several core features in their roles (i.e., frequent exposure to potentially traumatic events, high-stakes decision-making under pressure, and irregular work hours) and to combine them can simplify data collection and allow for generalized conclusions about PSP. However, distinctions between the two professions, such as the nature of exposure to trauma, public perception, organizational culture, and training may influence their psychological well-being and their attitudes toward seeking or accepting help (Carleton et al., 2018a). In this context, it is relevant to look at barriers and facilitators to help-seeking behaviour among police officers and firefighters considering the potential differences and similarities between these two professions. New findings will support the development of interventions designed to mitigate these barriers, tailored to the specific realities and needs of police officers and firefighters. The aim of this study is to provide a qualitative understanding of perceptions regarding seeking professional mental health support after being exposed to traumatic events at work (either from their own experience or through observations of their colleagues) in these two groups of PSP and identify potential differences between these two groups.
Research assistants recruited participants, throughout the province of Quebec, using a research poster, detailing the study’s objectives and contact information. It was shared in social media groups (Facebook) and posted in few police stations in Montreal, to enhance recruitment. Since firefighter participation through social media was sufficient, visiting fire stations to display the poster was unnecessary. The consent form was then sent by email. The project had ethical approval (CER-CEMTL 2020–2044) from the ethics committee of the Integrated University Health and Social Services Centre for the East Island of Montreal. No grants or funding sources were provided for this study. The interviews took place between March and August 2020. The interviews were conducted by telephone to optimize accessibility throughout the province of Quebec. Before the interview began, participants responded to a few sociodemographic questions. We used semi-structured interviews, from 30 to 60 minutes. The interview framework was developed based on open-ended questions about perception of self and general use of psychological help following a traumatic event (TE) at work (i.e., What do you personally do after experiencing a TE at work? In your opinion, do firefighters/police generally seek psychological help after a TE? Why or why not? What could be the effects of seeking help after a TE for firefighters/police?). Research assistants (two women, in their 30s, with a master’s degree in psychology and experiences in research interviews) conducted interviews in a quiet, confidential setting. For qualitative analysis purposes, the interviews were captured using a digital recorder, transcribed verbatim, and anonymized. Participants did not receive financial compensation, but they were provided with a list of mental health resources.
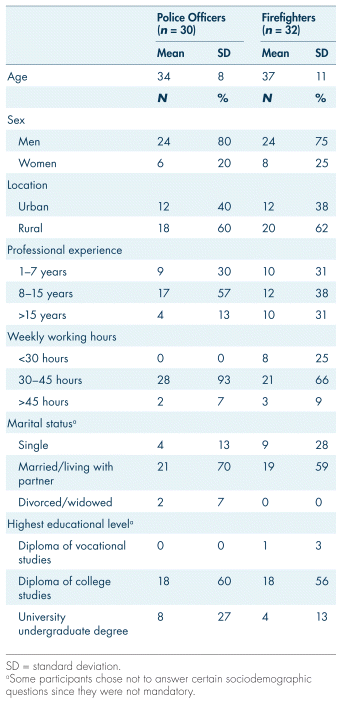
We recruited participants employed as police officers or firefighters across Quebec, Canada. Participants eligible for the study needed to be currently employed or have been out of work for less than 2 years. A minimum of 1 year of experience and fluency in French were required (interviews were conducted in French). We relied on participants’ self-reported exposure to TE that align with the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) criterion. This study followed the DSM-5 definition of TE for PTSD and acute stress disorder (criterion A), as it provides a widely recognized and standardized framework. We recognized that TE can be conceptualized in various ways. Participants were not required to disclose psychological disorders or prior mental health consultations, as the study focused on police and firefighters’ perceptions of seeking mental health support after workplace trauma. Given our limited resources of time and funds, we used convenience sampling (depending on the availability of participants) and maximum variation sampling (internal diversity) strategies (Moser & Korstjens, 2018). To achieve a sample representative of our research objectives, we aimed for adequate internal diversity based on several criteria: gender, age, location, years of experience, and weekly working hours (see Table I). The final sample comprised 62 participants. Drawing from the concept of information power (Malterud et al., 2016), we assessed that the information gathered was adequate (e.g., data redundancy) upon enrolling 30 police officers and 32 firefighters. According to information power principles, which consider factors such as study aims, sample specificity, existing theory, quality of dialogue, and analysis strategy, the depth of information reduced the need for additional participants. Importantly, all interviewed participants remained engaged throughout the study, with no dropouts.
TABLE I Participant demographic and professional information
The researchers who conducted the data analysis are a PhD student in psychology and an associate professor in nursing school, both specializing in the mental health of PSP. We conducted data analysis using an inductive thematic analysis approach as it allows researchers to identify, analyze, and report on patterns being data-driven and move away from a pre-existing coding framework and preconceptions to develop new knowledge of the topic at hand. Researchers followed the recommended six phases of thematic analysis: familiarizing with the data; generating preliminary codes; searching for potential themes; reviewing themes; defining and naming themes; and producing the report (Braun & Clarke, 2006; Nowell et al., 2017). The first author conducted an in-depth analysis of each interview to identify themes vertically. This was followed by a horizontal analysis across the entire sample to identify common themes and variations between interviews. The second author reviewed the suggested themes, and disagreements led to reexamining the data until the raters reached an agreement. Next, the two authors identified and discussed similarities and differences in the experiences within the contexts of police officers and firefighters. Given the substantial volume of data, the researchers utilized the QSR-NVivo V.12 software to assist in organizing, analyzing, and identifying relevant content within the qualitative data. This software facilitated coding, classification, and comparison of the material while preserving the researcher’s essential role in interpreting the data.
Our analysis revealed two distinct directions in the perceptions of our participants. Six themes were identified as barriers to seeking professional support among police officers and firefighters, while themes were found that could facilitate seeking such support (see Table II).
TABLE II Themes emerging from inductive thematic analysis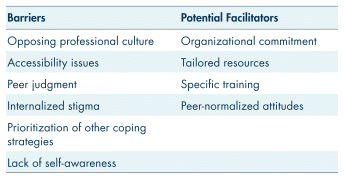
Several themes exhibit an organizational or systemic dimension, relying less on individual perspectives and more on characteristics of the existing system that appear to obstruct help-seeking behaviours.
Professional culture refers to a specific workplace ethos. In this context, it encompasses the beliefs, values, and attitudes derived from shared professional backgrounds that unite individuals in similar occupations with comparable training and field experience. Participants noted that seeking professional mental health support could potentially conflict with this professional culture.
While some participants acknowledged a shift and greater openness within police and firefighter cultures, the majority emphasized that certain aspects of these cultures can pose significant challenges to seeking or even considwwering professional mental health support after experiencing a TE. According to them, cultural values, such as the sense of sacrifice, fighting spirit, tenacity, pride, competitive drive, and strong desire to belong to a close-knit group, perpetuate the stigma surrounding mental health among many police officers and firefighters.
“The cultural perception is that you must be in control, and you must deal with every situation. You must be good at everything. You can’t be afraid; you must be a go-getter. You’ve got to go for the blows. But that means you can’t be vulnerable. You can’t project the image that you’re vulnerable.” (Police officer, PO-10)
“… quite similar people who have similar values in certain areas. At school, they’re taught to have a fireman’s mentality, a mentality of being afraid of nothing, a mentality of having confidence in yourself, of not showing weakness.” (Firefighter, F-17)
In addition to cultural values ingrained within the group, several participants expressed concern about seeking professional mental health support potentially harming their careers. They feared consequences such as being excluded from certain assignments by their supervisors, reassigned to different roles, suspended, or even terminated. They were also concerned about potential delays in promotions or being restricted from certain positions due to a history of mental health issues. Lastly, they feared that colleagues may become unwilling to work with them for safety reasons, or that they may be perceived as receiving preferential treatment from the organization. Overall, their concern was that seeking help, if known in the workplace, could be exploited against them professionally, potentially labelling them as a liability. This theme was much more prevalent among police participants (69% compared to 34%), suggesting that this concern is more prominent in their environment compared to firefighters.
“The risks of asking for help, there may be some police officers who will also be afraid that the employer will take over the case, then, you can lose your job, who can question our ability to do the work, then maybe dismiss us.” (PO-13)
Four participants distinctly noted active discouragement from the organizational hierarchy regarding seeking professional mental health support. This oppositional stance within the organization included discouraging employees from taking sick leave for psychological reasons or refusing to display promotional material about mental health. Consequently, employees seeking professional mental health support would be seen as going against their supervisors’ directives.
“The employer doesn’t really want us to get help, he doesn’t want us to miss work because of emotional problems. It’s more like denial.” (PO-5)
Participants highlighted numerous accessibility issues, which serve as practical barriers to seeking professional mental health support, even when individuals are motivated to seek help.
One of them was the lack of information on symptoms and treatments. Recognizing the need for help requires knowing how to identify the emergence and persistence of symptoms and being aware of the potential benefits of mental health support. However, our participants indicated that many police officers and firefighters lack knowledge about the symptoms that may arise after experiencing a TE, the potential benefits of therapy, the therapy process, its duration, and more. This lack of information prevented some of them from seeking support when they needed it.
“I didn’t know what the problem was. Before talking about it, I didn’t think I’d be traumatized on the job. It was clearly the specialists who helped me. For me, it was a lack of knowledge about my own health.” (PO-16)
Another area where information is lacking related to the process of accessing mental health services. Knowing whom to contact, how to reach them, which professionals are approved by the organization’s employee assistance program, what paperwork is required, and the steps involved were all aspects of the process that few seemed to understand. Some participants criticized their organizations for not clarifying this process adequately – for instance, by not offering information sessions or posting relevant details.
“There are also a lot of people who don’t know how to apply for help.” (F-23)
The complexity of the process for accessing support was also highlighted. They described the process of seeking appropriate support as excessively slow and complicated. For some, it had become a battle within the system to have their symptoms acknowledged as valid. The fear of facing pressure from insurance companies or their organization (i.e., needing to justify their symptoms, undergo a counter-assessment) led some individuals to consider it easier to continue working despite their symptoms rather than engaging in these complex and potentially invalidating procedures.
“It’s so heavy, asking for help. You know it’s not going to be easy, you know it’s going to be a problem with your peers, with human resources. It creates twice as much anxiety, when you know you have to get into it.” (PO-12)
Another accessibility issue appeared to be the lack of adapted resources. Participants expressed dissatisfaction with the limited coverage of therapy sessions by their employee assistance programs, the shortage of available mental health professionals, insufficient expertise among these professionals in trauma or the specific contexts of police and firefighter work, and the lack of early post-traumatic intervention to identify and promptly refer workers in need.
“I tried to get psychological help, and I was often referred by employee assistance, but the help wasn’t enough, in the sense that psychologists don’t really know anything about policing.” (PO-26)
The financial cost of seeking professional mental health support was also discussed. These concerns included the cost of additional sessions beyond those covered by the employee assistance program, expenses related to mental health professionals not covered by insurance, and potential reductions in pay during sick leave.
“You’re not covered at 100%. If I decide to go to the shrink because there’s something wrong with my job, I am covered for $500 a year. You can go 4 or 5 times. That’s a monthly rent after this. Depending on your financial situation, some guys might not be able to afford it.” (F-35)
Participants also identified the absence of guidance throughout the process as a significant barrier to accessibility. They highlighted concerns about having to initiate the first contact themselves during distress, encountering insufficient assistance with complex administrative procedures, and experiencing a lack of encouragement from managers to seek support.
“We’re told: ‘Well, go home, we’ll take care of everything’, but in reality, they don’t take care of anything. We don’t know what’s going on with our situation with human resources,… we don’t even know what paperwork we have to fill out.” (PO-12)
Finally, concern about confidentiality was mentioned in specific contexts. These included situations where individuals may need to go through their manager to access resource listings and in small communities where there are limited resources, making confidentiality harder to ensure.
“In a small village, if I go to see a shrink tomorrow morning, half of them know about it. We know the whole hospital. ‘What’s he doing in doctor x’s office?’ Smaller regions are less likely to seek help. That’s one reason not to go.” (PO-14)
Some participants noted positive shifts in colleagues’ attitudes toward the importance of mental health support for police officers or firefighters, indicating that certain work crews are more accepting than others. However, most participants reported that peer judgment remains a substantial obstacle, whether it is experienced firsthand or feared. Police officers reported this concern more frequently, although it is mentioned by a majority in both populations (96.5% compared to 81%). Two forms of peer judgment emerged in our interviews.
The fear of being perceived by colleagues or supervisors as too weak for the job appeared to be the most important concern regarding peer judgment. Police officers and firefighters worried about being mocked for seeking professional mental health support, whether related to the triggering event, the symptoms experienced, or their severity. Witnessing colleagues mock others for seeking support or taking sick leave, and fearing they will face similar ridicule themselves, appeared to deter some workers from seeking help when they need it.
“…fear of being judged by others. Fear of looking weak.” (F-1)
Another prevalent form of judgment was being perceived as exploiting the system by seeking mental health resources or requesting time off for recovery. Participants noted the greater controversy surrounding mental health-related absences compared to physical ones. They were concerned about being accused of lying about their condition, being labelled as lazy, or taking excessive vacation time. This aspect of peer judgment was exclusively reported by police officer participants; firefighters in our study did not mention this dimension of peer judgment.
“We’re going to associate people who seek help as they going to take advantage of the system. To be at home… everything post-traumatic and depression that we don’t see… the perception is that there are some who fake it and take advantage of the system… What I was thinking was ‘what are people going to say?’” (PO-10)
While certain barriers related to seeking professional mental health support after a work-related TE are rooted in organizational dynamics and require a systemic understanding, others appeared to be influenced by individual factors.
Stigma refers to negative perceptions or attitudes toward situations like experiencing symptoms after a TE at work. It often stems from others’ judgments but can also be internalized, where individuals apply negative stereotypes to themselves. Many of our participants associated seeking support for themselves with feelings of weakness or cowardice. They described how personal pride and ego can get in the way of seeking help. One of their explanations is that police and firefighters are typically seen as helpers in crisis situations. As individuals who typically assist others, they feel ashamed to seek help themselves. Some compared themselves to colleagues who are experiencing the same event but do not ask for help, while others compared themselves to civilians with mental health challenges whom they typically rescue, fearing being perceived similarly. These comparisons appeared to strengthen feelings of shame and a sense of losing status if they seek professional mental health support themselves. Although it was found in both populations, firefighter participants reported experiencing this internalized stigma more frequently (78% compared to 65.5%).
“Going to see a psychologist is perhaps cowardly and means not accepting the situation.” (F-20)
“People often call us when they’re at their wits’ end, they’ve got no resources left, and they often say, ‘You’re our saviors.’ By constantly being seen like that, guys with pride don’t want to show that they have weaknesses and that we’re human too, just like anyone else. So I’d say it’s really pride I think that’s going to play a part, hesitating to go and ask for help.” (F-23)
For some participants, seeking professional mental health support was viewed as a final resort among police officers and firefighters. They tended to prioritize alternative coping mechanisms, which range from adaptive to potentially more harmful. Both types were identified as substitutes for or delays in seeking professional mental health support and can therefore be considered as an obstacle.
Many participants commonly relied on social support as a coping strategy. They often mentioned turning to family members, typically spouses, or colleagues to discuss their challenges and release their emotions. For some, this approach seemed to replace the act of seeking professional mental health support.
“Usually, you will discuss the situation with trusted friends or family … The police usually do this with relatives.” (PO-36)
Another coping strategy mentioned by some participants involves trivialization, which includes making jokes, using dark humour, or laughing at the situation to manage and reduce psychological distress.
“I’ve never met a police officer who talked about something that affected him, except maybe as a joke.” (PO-16)
Avoidance was also a commonly employed coping strategy, manifesting in various forms such as trying to forget the intervention by moving on to the next call, disconnecting from one’s emotions voluntarily, using alcohol or drugs, engaging in distracting leisure activities to avoid thinking, or isolating oneself.
“You come back to the barracks on part-time duty, open a beer, take a shower, go home and that’s it.” (F-8)
Some participants pointed to a lack of self-awareness as a reason why police officers or firefighters may not seek professional mental health support promptly. They attributed this to a general lack of awareness regarding their own functioning and distress, a tendency to overlook internal changes, and a failure to recognize psychological damage following a TE.
“The person is either unaware or willfully blind to the fact that they need help. This is a phenomenon we’re going to see too. It’s a complete ignorance of the fact that the person has changed.” (PO-9)
Most of our participants expressed a clear and supportive attitude toward seeking professional mental health care after an overwhelming TE at work. Some highlighted the supportive role it plays in navigating difficult times, while others emphasized the positive impact on their professional identity and duties, such as remaining employed, effective, and competent. Many discussed the wider positive impact on their mental health and its effects on their personal and relational well-being. Our participants highlighted elements such as organizational commitment, tailored resources, specific training, and peer-normalized attitude that would encourage help-seeking among police officers and firefighters. These elements are described as either already in place or as anticipated and desired improvements.
Several participants highlighted the need for greater organizational commitment in seeking mental health support. This is mentioned more frequently in interviews with police officers than with firefighters (48% compared to 34%). For these participants, the organization should take a more proactive role in providing information about professional mental health support, supervisors should receive specialized training to better identify individuals showing symptoms and know how to respond, and the organization should support employees throughout the process of seeking mental health support. Some believed that mental health support should be automatically offered by managers after high-risk interventions, or that regular sessions should be mandatory throughout a career. They argued that employees are more likely to accept help when it is offered to them than to seek it out independently. In their view, it would be more effective for the organization to initiate the request for help rather than placing the responsibility on the struggling employee.
“When you’re exposed to a traumatic event, in my opinion there should automatically be a consultation with one of the support programs. We shouldn’t wait until someone is in distress and then ask for help. A quick half-hour meeting, which is mandatory afterwards, I think could perhaps avoid future problems.” (F-23)
A very frequent theme highlighted by participants is the need to optimize available resources to better meet their needs. They discussed various aspects of how these resources could be tailored to be more effective.
Participants requested that support resources be specialized and well-versed in the tasks and culture of PSP to enhance workers’ trust in seeking support. They proposed several improvements, including using peer helpers who understand the workplace to assist with screening and encourage initial help-seeking. Some suggested having mental health professionals stationed directly at each police station or fire department, with a permanent office in these locations, fostering trust. Additionally, they recommended that the mental health professionals listed in the employee assistance program be chosen for their expertise in trauma and their familiarity with the workplace.
“To call into a help center that has been contracted with the city. They know that if someone calls and it’s a firefighter, it’s been negotiated and we know it’s an emergency service worker, so the help is more specialized than general.” (F-7)
Enhancing the visibility of available resources is also highlighted as a factor that could encourage support-seeking. This could involve increased promotion of mental health support resources within the organization, regular reminders from managers, and signage in various locations such as stations and vehicles.
“Let it be seen maybe with posters, but let it really be known and clear that this is the way we do things. That would make things a lot easier.” (F-16)
They also recommended extending the duration and variety of available resources. This could involve increasing the number of sessions covered by the employee assistance program and broadening the types of therapies offered to address specific challenges faced by police officers and firefighters.
“Eight one-hour meetings went by fast. Open up the resource more, open up more sessions. This could be better perceived by members.” (PO-11)
The problem of delays in receiving support was also highlighted. Participants noted that a shorter wait time between requesting and receiving support would be more motivating for PSP. They suggested aiming for a maximum delay of 24 hours, providing 24/7 coverage, or establishing a hotline.
“See a 24-hour maximum delay before being seen, because you know, often when a policeman asks for help, well, it’s already too late.” (PO-19)
Finally, some participants highlighted the need to simplify the support-seeking process. They advocated for a clearer, more user-friendly procedure, such as a pre-established protocol, a reduction in administrative tasks, or guidance throughout the process.
“To facilitate the whole process, it’s essential, because if it’s complicated, it just adds to the pile.” (PO-19)
Several participants requested specific training on mental health and symptoms that can develop after exposure to TE. They recommended including this during their initial training with an emphasis on prevention. Periodic follow-up training was also suggested. Additionally, some participants proposed offering training to relatives to help them identify changes in the exposed worker.
“At school, for example, we have a psychological health course. It was a 40-hour course dedicated to ‘What can you do in a stressful situation? How do you deal with post-traumatic shock? What to do if your colleague experiences it?’. So already the fact that he’s giving a course at school, I think it’s great.” (F-33)
“Raising awareness among family and friends.” (PO-26)
Several participants highlighted the importance of positive narratives from colleagues who have experienced post-traumatic symptoms and sought support. They stated that being surrounded and supported by receptive and understanding colleagues would encourage more police officers and firefighters to seek support. They advocated for mutual vigilance in identifying needs. Police officers reported peer-normalized attitudes as a potential facilitator much more frequently than firefighters (48% compared to 22%).
“I think what would be most effective… It has to come from the police themselves. Those who have sought help, let them explain what led them to seek help. How they felt before, during and after.” (PO-10)
Increasingly, studies are examining PSP mental health and the barriers to seeking support, a topic that has long been taboo for these workers (Haugen et al., 2017). To better understand subjective and individual experiences, we employed an inductive thematic analysis in this study. Themes were identified and organized, revealing both barriers and potential facilitators to mental health support among police officers and firefighters. Some themes were more prevalent within specific groups. Although unintentional, the facilitators suggested by participants often mirror the identified barriers. Therefore, we have chosen to present them together in this section, aiming to enhance the reader’s understanding.
One of the main barriers was the theme of opposing professional culture. Participants highlighted aspects of this culture that perpetuate the stigma surrounding mental health for most PSP. From the three identified sub-themes, opposed cultural values are also recognized by other studies. Drew and colleagues (2021) found that 65.4% of police participants in the United States identified overall cultural stigma about behavioural mental health as a barrier to seeking help. The second sub-theme, detrimental impacts on their career, is also highlighted in recent literature. Police officers and firefighters worry that seeking professional mental health support could jeopardize their jobs or negatively impact their careers (Drew & Martin, 2021; Haugen et al., 2017; Newel et al., 2022).
The third sub-theme, organizational opposition, highlighted how the organization can actively perpetuate barriers and adversely affect support-seeking behaviour. This element is less commonly found in the literature, though it can be related to Ricciardelli’s work on structural factors that amplify mental health stigma, hinder awareness, and create obstacles to care for Canadian PSP (Ricciardelli et al., 2018). As a potential facilitator, the theme, organizational commitment, directly addresses the previous barriers and highlights the role of professional culture in driving positive change. Participants acknowledged that an increase in organizational commitment is essential to encouraging the pursuit of mental health support among PSP, a view supported by several studies (Hofer & Savell, 2021; Tucker, 2015).
Accessibility issues were another major barrier. Participants identified several practical obstacles. Most of them align with findings from earlier studies on the topic, such as the lack of information regarding the process of accessing help (Haugen et al., 2017), the complexity of the process (Haugen et al., 2017), the lack of adapted resources (Drew & Martin, 2021; Gulliver et al., 2019), and the concern for confidentiality (Haugen et al., 2017; Newel et al., 2022; Tucker, 2015). Our participants also highlighted issues such as lack of information regarding symptoms and treatments, the financial costs associated with professional mental health support, and a lack of guidance throughout the help-seeking process. These accessibility concerns seem to add new insights to the existing literature. In response, participants suggested potential facilitators related to tailored resources that enhance accessibility. Some of these aspects align with previous research, such as the need for resources specialized in PSP culture (Gulliver et al., 2019; Hofer & Savell, 2021; Newel et al., 2022), improving the visibility of available resources (Newel et al., 2022), and simplifying the help-seeking process (Hofer & Savell, 2021; Newel et al., 2022). Some suggestions for tailoring resources such as increasing the duration and diversity of available resources and reducing the time between requesting and receiving help seem to be novel contributions to the literature on this topic.
Despite significant progress, participants also recognized that peer judgment continues to be an obstacle. They identified two specific forms of judgment from their colleagues. The perception of being deemed too weak for the job is well-documented in recent literature (Drew & Martin, 2021; Gulliver et al., 2019; Haugen et al., 2017; Kim et al., 2018; Newel et al., 2022). Additionally, participants noted concerns about being perceived as exploiting the system, a theme also observed in studies (Gulliver et al., 2019; Haugen et al., 2017; Kim et al., 2018; Ricciardelli et al., 2018; Tucker, 2015). Building on the impact of peer perceptions, our participants identified peer-normalized attitudes as a facilitator for seeking mental health support. They emphasized that beyond merely avoiding judgment, having colleagues who actively watch out for each other, share positive narratives, and offer guidance would significantly boost their willingness to seek help. There is no known research that has focused on this topic.
Internalized stigma was another barrier identified by our participants. Previous studies often merge external stigma with internalized stigma (Gulliver et al., 2019; Haugen et al., 2017; Kim et al., 2018; Tucker, 2015). However, based on participants’ insights, it is crucial to distinguish between these two forms. Internalized stigma often originates from peer judgments, but it can persist even in the absence of such judgments.
According to our participants, prioritizing other coping strategies can be seen as an additional barrier to seeking professional support. The notion that coping mechanisms like social support, trivialization, or avoidance of symptoms might be used to replace or postpone seeking professional support seems to be relatively novel in the literature although Syed and colleagues (2020) addressed maladaptive coping strategies as risk factors for mental health issues among police personnel.
Finally, a lack of self-awareness about post-traumatic symptoms or behavioural changes was identified as an additional barrier. In contrast, participants emphasized the value of specific training on this subject to improve mental health help-seeking. They requested training on mental health and specific post-traumatic symptoms during their initial training and periodic follow-up sessions. Additionally, they proposed offering this training to relatives to assist them in recognizing changes. Prevention of psychological issues for PSP is a widely discussed topic in the literature (Hofer & Savell, 2021; Lu & Petersen, 2023; Wild et al., 2020), though evidence supporting its effectiveness is still developing.
Several researchers have expressed concern about treating all PSP as a uniform group and providing them with a one-size-fits-all response (Carleton et al., 2018a; Klimley et al., 2018). They recommend considering occupation-specific perspectives and addressing differences to offer responses tailored to their specific needs and characteristics. In our study, although the obstacles and facilitators applied to both police officers and firefighters, the frequency of certain themes differed.
Regarding obstacles, fears about detrimental impacts on their career were more prevalent among police officers than firefighters. This could be partly explained by the fact that legal concerns are more prevalent among police officers than firefighters. Consequently, police officers might be more reluctant to admit to mental health problems and seek help, as they fear this could be used against them if investigative measures are initiated. Police officers reported more peer judgment, while firefighters reported more internalized stigma. This suggests that police officers are more concerned about external reactions to their mental health, aligning with their fear of workplace repercussions. Differences in recruit training may also explain variations in internalized stigma, as police officers often receive more mental health education than firefighters.
Regarding facilitators, police officers, who experienced more peer judgment, were more likely than firefighters to highlight peer-normalized attitudes as a key factor in encouraging mental health support-seeking. Similarly, police officers placed greater emphasis on the role of organizational commitment in promoting support-seeking behaviour. Tucker’s (2015) article explored the role of perceived organizational support in encouraging police officers to use stress intervention services. We can hypothesize that police officers may need organizational changes to increase support-seeking behaviours. This issue is less common among firefighters, possibly because they are at an earlier stage of change and have not yet encountered the same organizational barriers. Also, police officers are typically full-time employees, while firefighters in Quebec may work part-time and have additional careers. This difference can lead to less organizational pressure on firefighters and more emphasis on personal aspects of seeking help. These observations are preliminary, and further studies, including quantitative research, are necessary to confirm whether these differences are consistent and generalizable.
While methodological choices such as telephone and individual interviews facilitated recruitment and ensured confidentiality, they also risked missing out on certain information, such as non-verbal cues and group dynamics, which can be considered a limitation. Another limitation is the potential non-participation of individuals with higher mental health stigma, who may have been unwilling to participate. Furthermore, our recruitment strategy has missed individuals on leave due to a mental disorder, potentially limiting the richness of the data.
This study employs a qualitative analysis approach. While our results are not meant for broad generalization, we believe they offer satisfying transferability due to the sample size and adherence to the principles of information power (Malterud et al., 2016). On another note, this study focused exclusively on French-speaking police officers and firefighters in the province of Quebec. French-speaking PSP are not represented in a large contingent of the research done on PSP mental health in Canada, with studies focusing only on English-speaking PSP frequently. Additional research is required to determine how far these findings can be transferrable to non-French-speaking PSP and PSP in other sectors (Ahmed, 2024). Ultimately, our study provides detailed insights into both barriers and facilitators, which supports the practical application of research findings (see Table III).
TABLE III Key recommendations based on the research results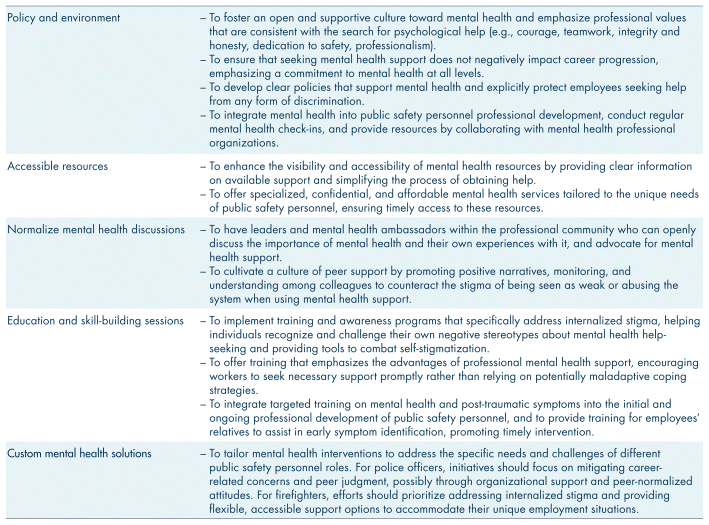
Enhanced mental health care for PSP benefits not only the individuals themselves but also their families, colleagues, and the communities they serve. This study offers a qualitative look at police and firefighters’ perceptions of seeking mental health support after TE at work. It highlights barriers and suggests improvements through organizational commitment, tailored resources, specific training, and peer-normalized attitudes. Understanding these factors can guide organizations in supporting their employees and adapting practices to the specific needs of each group. Future research should broaden the scope to include additional PSP and employ a comparative approach to enhance our understanding of the unique needs of each profession. This will assist in addressing both individual and systemic barriers and ensuring suitable support for these high-risk workers.
The researchers would like to thank the police officers and firefighters who participated in this study as well as the research assistants Caroline Bellegy and Marie-Astrid Traeger.
No grants or funding was provided for this study.
The authors have no conflicts of interest to declare.
The project had ethical approval (CER-CEMTL 2020–2044) from the ethics committee of Integrated University Health and Social Services Centre for the East Island of Montreal.
There is no previous or duplicate publication.
*Department of Psychology, Université de Montréal, QC, Canada;
†Trauma Studies Center, University Institute of Mental Health of Montreal, QC, Canada;
‡School of Nursing, Université de Montréal, QC, Canada.
Ahmed, S. K. (2024). The pillars of trustworthiness in qualitative research. Journal of Medicine, Surgery, and Public Health, 2, 100051. https://doi.org/10.1016/j.glmedi.2024.100051
Crossref
Bernier, L. (2021). Stigmate public et barrières à la consultation: Étude sur des facteurs pouvant influencer l’utilisation des services d’aide psychologique chez les policiers et les policières. [Thèse de doctorat, Université de Sherbrooke]. SavoirU Sherbrooke. https://savoirs.usherbrooke.ca/handle/11143/19195
Boivin, B. D., Boudreault, P. (2022). Système de gestion des risques liés à la fatigue pour les policiers en autopatrouille (Rapport n° R-1131-fr). IRSST. www.irsst.qc.ca/media/documents/PubIRSST/R-1131-fr.pdf
Braun, V., Clarke, V. (2006). Using thematic analysis in psychology. Qualitative Research in Psychology, 3(2), 77–101. https://doi.org/10.1191/1478088706qp063oa
Crossref
Carleton, R. N., Afifi, T. O., Turner, S., Taillieu, T., Duranceau, S., LeBouthillier, D. M., Sareen, J., Ricciardelli, R., MacPhee, R. S., Groll, D., Hozempa, K., Brunet, A., Weekes, J. R., Griffiths, C. T., Abrams, K. J., Jones, N. A., Beshai, S., Cramm, H. A., Dobson, K. S., … Asmundson, G. J. G. (2018a). Mental disorder symptoms among public safety personnel in Canada. Canadian Journal of Psychiatry, 63(1), 54–64. https://doi.org/10.1177/0706743717723825
Crossref
Carleton, R. N., Afifi, T. O., Turner, S., Taillieu, T., LeBouthillier, D. M., Duranceau, S., Sareen, J., Ricciardelli, R., MacPhee, R. S., Groll, D., Hozempa, K., Brunet, A., Weekes, J. R., Griffiths, C. T., Abrams, K. J., Jones, N. A., Beshai, S., Cramm, H. A., Dobson, K. S., … Asmundson, G. J. G. (2018b). Suicidal ideation, plans, and attempts among public safety personnel in Canada. Canadian Psychology, 59(3), 220–231. https://doi.org/10.1037/cap0000136
Crossref
Carleton, R. N., Korol, S., Mason, J. E., Hozempa, K., Anderson, G. S., Jones, N. A., Dobson, K. S., Szeto, A., Bailey, S. (2018c). A longitudinal assessment of the road to mental readiness training among municipal police. Cognitive Behaviour Therapy, 47(6), 508–528. https://doi.org/10.1080/16506073.2018.1475504
Crossref
Chopko, B. A., Palmieri, P. A., Facemire, V. C. (2014). Prevalence and predictors of suicidal ideation among U.S. law enforcement officers. Journal of Police and Criminal Psychology, 29(1), 1–9. https://doi.org/10.1007/s11896-013-9116-z
Crossref
Chu, C., Buchman-Schmitt, J. M., Hom, M. A., Stanley, I. H., Joiner, T. E. (2016). A test of the interpersonal theory of suicide in a large sample of current firefighters. Psychiatry Research, 240, 26–33. https://doi.org/10.1016/j.psychres.2016.03.041
Crossref PubMed PMC
Drew, J. M., Martin, S. (2021). A national study of police mental health in the USA: Stigma, mental health and help-seeking behaviors. Journal of Police and Criminal Psychology, 36(2), 295–306. https://doi.org/10.1007/s11896-020-09424-9
Crossref
Edgelow, M., Fecica, A., Kohlen, C., Tandal, K. (2023). Mental health of public safety personnel: Developing a model of operational, organizational, and personal factors in public safety organizations. Frontiers in Public Health, 11, 1140983. https://doi.org/10.3389/fpubh.2023.1140983
Crossref PubMed PMC
Encrenaz, G., Miras, A., Contrand, B., Séguin, M., Moulki, M., Queinec, R., René, J.-S., Fériot, A., Mougin, M., Bonfils, M., Marien, P., Michel, G., Lagarde, E. (2016). Suicide dans la police nationale Française: Trajectoires de vie et facteurs associés. L’Encéphale, 42(4), 304–313. https://doi.org/10.1016/j.encep.2015.08.004
Crossref
Geoffrion, S., Leduc, M.-P., Bourgouin, E., Bellemare, F., Arenzon, V., Genest, C. (2023). A feasibility study of psychological first aid as a supportive intervention among police officers exposed to traumatic events. Frontiers in Psychology, 14, 1149597. https://doi.org/10.3389/fpsyg.2023.1149597
Crossref PubMed PMC
Government of Canada. (2016). Supporting Canada’s public safety personnel: An action plan on post-traumatic stress injuries. Public Safety Canada. https://www.publicsafety.gc.ca/cnt/rsrcs/pblctns/2019-ctn-pln-ptsi/index-en.aspx
Gulliver, S. B., Pennington, M. L., Torres, V. A., Steffen, L. E., Mardikar, A., Leto, F., Ostiguy, W., Zimering, R. T., Kimbrel, N. A. (2019). Behavioral health programs in fire service: Surveying access and preferences. Psychological Services, 16(2), 340–345. https://doi.org/10.1037/ser0000222
Crossref
Haugen, P. T., McCrillis, A. M., Smid, G. E., Nijdam, M. J. (2017). Mental health stigma and barriers to mental health care for first responders: A systematic review and meta-analysis. Journal of Psychiatric Research, 94, 218–229. https://doi.org/10.1016/j.jpsychires.2017.08.001
Crossref PubMed
Hofer, M. S., Savell, S. M. (2021). “There was no plan in place to get us help”: Strategies for improving mental health service utilization among law enforcement. Journal of Police and Criminal Psychology, 36(3), 543–557. https://doi.org/10.1007/s11896-021-09451-0
Crossref
Johnson, C. C., Vega, L., Kohalmi, A. L., Roth, J. C., Howell, B. R., Van Hasselt, V. B. (2020). Enhancing mental health treatment for the firefighter population: Understanding fire culture, treatment barriers, practice implications, and research directions. Professional Psychology: Research and Practice, 51(3), 304–311. https://doi.org/10.1037/pro0000266
Crossref
Jones, S., Agud, K., McSweeney, J. (2020). Barriers and facilitators to seeking mental health care among first responders: “Removing the darkness”. Journal of the American Psychiatric Nurses Association, 26(1), 43–54. https://doi.org/10.1177/1078390319871997
Crossref
Kim, J. E., Dager, S. R., Jeong, H. S., Ma, J., Park, S., Kim, J., Choi, Y, Lee, S. L., Kang, I., Ha, E., Cho, H. B., Lee, S., Kim, E. J., Yoon, S., Lyoo, I. K. (2018). Firefighters, posttraumatic stress disorder, and barriers to treatment: Results from a nationwide total population survey. PLoS One, 13(1), e0190630. https://doi.org/10.1371/journal.pone.0190630
Crossref PubMed PMC
Klimley, K. E., Van Hasselt, V. B., Stripling, A. M. (2018). Posttraumatic stress disorder in police, firefighters, and emergency dispatchers. Aggression and Violent Behavior, 43, 33–44. https://doi.org/10.1016/j.avb.2018.08.005
Crossref
Lu, Y. F., Petersen, K. (2023). Effectiveness of psychological skills training for police personnel: A meta-analysis. Occupational and Environmental Medicine, 80(10), 590–598. https://doi.org/10.1136/oemed-2023-109117
Crossref PubMed
Malterud, K., Siersma, V. D., Guassora, A. D. (2016). Sample size in qualitative interview studies: Guided by information power. Qualitative Health Research, 26(13), 1753–1760. https://doi.org/10.1177/1049732315617444
Crossref
Moser, A., Korstjens, I. (2018). Series: Practical guidance to qualitative research. Part 3: Sampling, data collection and analysis. The European Journal of General Practice, 24(1), 9–18. https://doi.org/10.1080/13814788.2017.1375091
Crossref
Newel, C. J., Ricciardelli, R., Czarnuch, S. M., Martin, K. (2022). Police staff and mental health: Barriers and recommendations for improving help-seeking. Police Practice Research: An International Journal, 23(1), 111–124. https://doi.org/10.1080/15614263.2021.1979398
Crossref
Nowell, L. S., Norris, J. M., White, D. E., Moules, N. J. (2017). Thematic analysis: Striving to meet the trustworthiness criteria. International Journal of Qualitative Methods, 16, 1–13. https://doi.org/10.1177/1609406917733847
Crossref
Quarshie, E. N., Odame, S. K., Annor, F. (2021). Suicidal behaviors in the Ghana Police Service. Crisis, 42(3), 194–201. https://doi.org/10.1027/0227-5910/a000707
Crossref
Ricciardelli, R., Carleton, R. N., Mooney, T., Cramm, H. (2018). “Playing the system”: Structural factors potentiating mental health stigma, challenging awareness, and creating barriers to care for Canadian public safety personnel. Health (London, England: 1997), 24(3), 259–278. https://doi.org/10.1177/1363459318800167
Crossref
Syed, S., Ashwick, R., Schlosser, M., Jones, R., Rowe, S., Billings, J. (2020). Global prevalence and risk factors for mental health problems in police personnel: A systematic review and meta-analysis. Occupational and Environmental Medicine, 77(11), 737–747. https://doi.org/10.1136/oemed-2020-106498
Crossref PubMed
Tucker, J. M. (2015). Police officer willingness to use stress intervention services: The role of perceived organizational support (POS), confidentiality and stigma. International Journal of Emergency Mental Health and Human Resilience, 17(1), 304–314. Retrieved from htteps://digitalcommons.wcupa.edu/crimjust_facpub/4
Wild, J., Greenberg, N., Moulds, M. L., Sharp, M.-L., Fear, N., Harvey, S., Wessely, S., Bryant, R. A. (2020). Pre-incident training to build resilience in first responders: Recommendations on what to and what not to do. Psychiatry: Interpersonal and Biological Processes, 83(2), 128–142. https://doi.org/10.1080/00332747.2020.1750215
Crossref
Correspondence to: Marine Tessier, Centre d’étude sur le trauma, CRIUSMM, 7331, rue Hochelaga, Montréal, QC H1N 3V2, Canada. Telephone: +1-514-251-4015., E-mail: tessier.marine@gmail.com
This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/. For commercial re-use, please contact sales@sgpublishing.ca.
Journal of CSWB, VOLUME 10, NUMBER 3, September 2025