Sebastian Harenberg*, Michelle C. E. McCarron†, Margaret Nieto*, Owen Scheirer‡, R. Nicholas Carleton¶, Terence Ross‡
ABSTRACT
Emergency services personnel are regularly exposed to potentially traumatic events with substantial consequences for their mental health. Current estimations from Canadian emergency medical service (EMS) providers show a prevalence of clinically relevant symptomology of 20% or higher in anxiety, depression, and post-traumatic stress. Interestingly, evidence from Canadian helicopter emergency medical services (HEMS) demonstrates a substantially lower prevalence rate (i.e., <10%) of mental disorder symptoms. However, current Canadian data stem from a single HEMS service. A comprehensive assessment of mental disorders from a larger, nationwide sample is presently absent, which was the purpose of the current study. A sample of 215 HEMS personnel (male n = 165, 76.6%) from six Canadian provinces (AB, BC, SK, MB, ON, NS) completed an online survey measuring several mental disorder symptoms. The results revealed a prevalence of clinically elevated symptoms of 7% in posttraumatic stress disorder, 16.8% in major depressive disorder, 5.6% in anxiety, and 3.7% stress. Paramedics reported a significantly higher prevalence of clinically elevated symptoms of post-traumatic stress disorder and major depressive disorder symptoms compared to other HEMS personnel. The findings indicate a higher prevalence of some mental disorder symptoms (i.e., post-traumatic disorder, major depressive disorder) compared to existing data from a single Canadian HEMS organization. There are several psychological (e.g., coping mechanisms), organizational (e.g., time for structured debriefing), and extraneous factors (e.g., COVID-19 pandemic) that may have influenced the results. Yet, the prevalence levels remain much below those reported in on-the-ground EMS workers, which warrants further investigation.
Key Words Mental health; first responders; helicopter emergency medical services; PTSD.
Emergency medical service (EMS) personnel (e.g., physicians, nurses, paramedics, pilots) work in highly dynamic environments, which expose them to unpredictable and potentially psychologically traumatic events (PPTEs, which consist of actual or threatened death, serious injury, or sexual violence; APA, 2022) much more frequently than would be expected for the general public (Carleton et al., 2019; CIPSRT, 2019). The stressors may negatively impact physiological responses (e.g., heart rate variability; Petrowski et al., 2023) and well-being, as well as lead to an increase in the prevalence of mental disorders among EMS personnel (Lawn et al., 2020). A recent meta-analysis (Petrie et al., 2018) estimated the prevalence of post-traumatic stress disorder (PTSD) and other mental disorders in ambulance personnel at more than 10%. Canadian data suggest over one in five EMS workers reported elevated symptoms for major depressive disorder (29.6%), PTSD (24.5%), and social anxiety disorder (20%, Carleton et al., 2018). Taken together, current evidence highlights the immense emotional burden of working in paramedicine.
In helicopter emergency medical services (HEMS), personnel engage in PPTEs in a particularly complex fashion (e.g., attending to severe accidents, events of life-threatening injuries, severe pediatric cases) as a function of transport using helicopters. HEMS personnel missions typically involve PPTEs with a high chance of mortality. Long transportation times from rural communities and changes in weather can further complicate missions and serve as added stressors on HEMS personnel. Despite the additional stressors, research examining mental disorder symptoms among HEMS personnel showed much lower prevalence compared to on-the-ground emergency health care professionals (Carleton et al., 2018). For example, Reid et al. (2022) collected data from 161 Norwegian HEMS personnel evidencing positive screening prevalence proportions for PTSD of 3.9%, and for major depressive disorder and generalized anxiety of 1.9%.
The first study assessing mental disorder symptoms in Canadian HEMS personnel involved 100 participants from a single air ambulance service in mid-Western Canada (Harenberg et al., 2018). There were 5% of participants who screened positive for clinically elevated symptoms of PTSD, which was comparable to the general population (i.e., 3.5–6.8%; Kessler et al., 2005) and the Norwegian sample (Reid et al., 2022), but lower than a national Canadian paramedic sample (i.e., 24.5%; Carleton et al., 2018). The prevalence of clinically significant screens for depression symptoms (i.e., 3%), anxiety symptoms (i.e., 9.1%), and stress (i.e., 16.5%) were also lower in the Canadian HEMS personnel sample (Harenberg et al., 2018) than for the national Canadian paramedic sample (Carleton et al., 2018); however, the studies differed in the measures to assess the symptoms of depression, anxiety, and stress.
The current HEMS personnel mental health research used relatively small sample sizes from single organizations, limiting the generalizability of results; nevertheless, the differences relative to extant paramedic research suggest that, pending additional evidence, there may be important differences between HEMS personnel and on-the-ground emergency health care professionals that may warrant attention from researchers, clinicians, and policymakers. Before such exploration may be undertaken, data from nationally representative samples ought to be collected. Hence, the current study was designed to assess the prevalence of clinically significant mental disorder symptoms in a large sample of Canadian HEMS personnel.
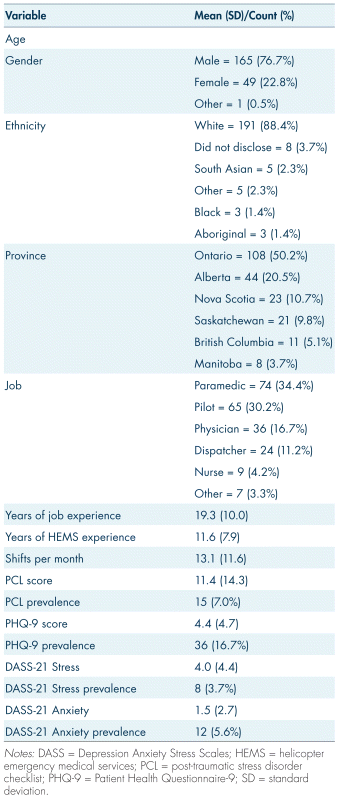
There were 215 HEMS personnel from six Canadian provinces (AB, BC, SK, MB, ON, NS) who participated in the current study. Most participants were male (n = 165; 76.7%) and identified as white (n = 191; 88.8%). Participants had an average of 19.2 (standard deviation (SD) = 10.0) years of job experience, 11.6 (SD = 7.9) years of HEMS experience, and took 13.1 (SD = 11.6) HEMS shifts per month. Most participants worked as paramedics (n = 74; 34.4%), pilots (n = 65; 30.2%), physicians (n = 36; 16.7%), dispatchers (n = 24; 11.2%), nurses (n = 9; 4.2%), or other staff (n = 7; 3.3%).
The current study was approved by the ethics board of the Saskatchewan Health Authority (REB-20-09) and conducted with permission of the participating HEMS organizations. The design and reporting followed the consensus-based checklist by Sharma et al. (2021). The link to an anonymous online survey was shared with the HEMS organizations for distribution via internal e-mail addresses. The participants indicated their consent to the study by completing the survey. Demographic information and mental health symptoms (i.e., PTSD, major depressive disorder, anxiety, and stress) were collected.
The PTSD checklist (PCL-5; Blevins et al., 2015) assesses PTSD symptoms on 20 items, which are rated using a Likert-type scale ranging from 0 (not at all) to 4 (extremely). A total severity score (i.e., sum of all items) was used for the current study. Following the DSM-5, participants were flagged for clinically meaningful PTSD symptoms if they showed a severity score > 33 and elevated responses (i.e., 2 or higher) in all segments of the PCL-5. Good internal consistency was also observed in the present study (Cronbach’s α = 0.96).
The Patient Health Questionnaire-9 (PHQ-9, Kroenke et al., 2001) was used to assess symptoms of major depressive disorder. The nine items are scored on a Likert scale ranging from 0 (not at all) to 3 (nearly every day). A total severity score (i.e., sum of all items) was used for the current study, with a score of 10 or above indicating clinically meaningful major depressive disorder symptoms. The internal consistency of the scale in the present study was satisfactory (Cronbach’s α = 0.88).
The anxiety and stress subscales of the Depression Anxiety Stress Scales (DASS-21, Lovibond & Lovibond, 1995) were used. The seven items for each subscale are scored on a Likert scale ranging from 0 (never) to 3 (almost always). A total severity score (i.e., sum of all items) was used for the current study, with a score of >7 for anxiety and >14 for stress indicating clinically meaningful symptoms (i.e., mild or above). The internal consistency of both subscales was satisfactory (Cronbach’s α > 0.85).
Categorical variables were summarized in counts and percentages, while continuous variables were aggregated in means and standard deviations. Chi-squared tests with Fisher’s correction (where applicable) were used to compare categorical variables. For continuous variables, bivariate Pearson correlations were calculated to assess the relationship between measures. Independent t-tests with Cohen’s d or oneway analysis of variance with partial eta-squared effect sizes were calculated to compare differences between professional groups within HEMS (e.g., pilots, physicians, paramedics, dispatchers). If assumptions (e.g., normality) were violated, non-parametric analyses were used. All analyses were conducted in JASP 0.17.2 and a significance level of 0.05 was set.
The descriptive and demographic information are reported in Table I. There were 15 participants who screened positively for clinically elevated symptoms of PTSD (7%). In addition, 36 participants screened positively for clinically elevated symptoms of major depressive disorder (16.8%) and anxiety (n = 12; 5.6%), and 8 participants showed elevated stress (3.7%). All self-reported symptom scores were inter-correlated and reported in Table II.
TABLE II Correlations of mental health variables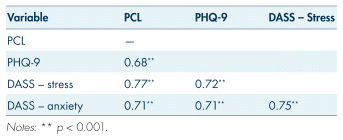
There were statistically significant differences across job types for symptoms of PTSD, F(5,208) = 5.38, p < 0.001, η2p = 0.11, as detailed in Table III. Paramedics reported statistically significantly higher levels of PTSD symptoms compared to other subgroups. Paramedics also reported significantly higher symptoms of major depressive disorder, F(5,208) = 3.45, p < 0.001, η2p = 0.08, and statistically significantly higher proportion of positive screenings for major depressive disorder compared to other job types (27.0%, χ2 = 12.74, p = 0.026, Cramer’s V = 0.24). For the remaining variables, there were no other statistically significant differences between job types. There were also no statistically significant differences based on other demographic categories (see Table III).
TABLE III Mental disorder symptoms by job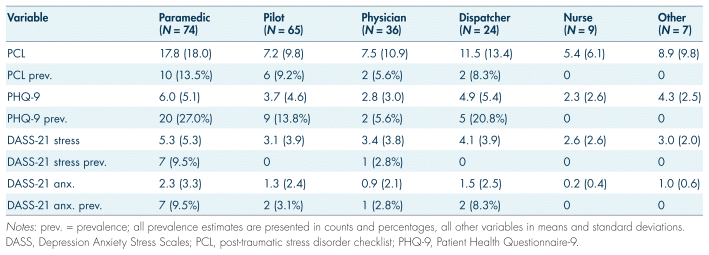
The purpose of the present study was to examine the symptoms of mental disorders in Canadian HEMS personnel. Nationally and internationally, the well-being and mental health in this population is understudied. Only a single study with a Canadian HEMS sample exists (Harenberg et al., 2018), suggesting a low prevalence of symptoms of post-traumatic stress, depression, anxiety, and stress. Yet, these data were collected from 100 participants in a single Canadian HEMS organization. The present study is a national-level update from six Canadian provinces with a substantially larger sample size. The current findings suggest a higher prevalence of elevated post-traumatic stress and depressive symptoms than indicated by previous data.
The prevalence of clinically elevated symptoms of post-traumatic stress in the current sample was 9.4%, which is substantially higher than a previous Canadian prevalence study (i.e., 5%; Harenberg et al., 2018) and more than double of the prevalence found in a study from Norway (i.e., 3.9%; Reid et al., 2022). Accordingly, the prevalence of clinically elevated symptoms of major depressive disorder in the present study was also much higher (16.8%) compared to existing HEMS studies. The most obvious explanation for both findings would be that the data from this study were collected during the COVID-19 pandemic, which forced HEMS personnel to be in close spaces with infected patients for long durations. The fear of potential infection and long absence of pre-hospital guidelines on how to safely transport COVID patients (Albrecht et al., 2020) may have aggravated some mental disorder symptoms. Another explanation could be the administration of the online survey. In the study by Harenberg et al. (2018), e-mails were sent from a researcher who was also affiliated with the HEMS organization. This may have jeopardized the sense of anonymity for some participants, potentially leading to more socially desirable answers (i.e., underreporting of symptoms). In the present study, e-mails were sent from an unaffiliated account and clearly mentioned a principal investigator outside of any HEMS organization, which may have fostered a sense of anonymity for the responses of the participants.
Paramedics in the present study experienced significantly higher rates of post-traumatic stress and symptoms of depression compared to the other professional groups in HEMS. Previous research identified organizational factors (e.g., lack of safety particularly during COVID-19, Petrie et al., 2022), environmental factors (e.g., rural care, Courtney et al., 2013), and psychological factors (e.g., burnout, Reardon et al., 2020), among others that may negatively influence paramedics’ well-being. For the present study, the paramedics were part of the same organizations and missions as other staff (e.g., physicians). As such, some of the environmental or organizational stressors could be excluded as possible reasons as they were the same for several subgroups of participants. However, in contrast to HEMS physicians and other staff, some of the HEMS paramedics might have also been involved in regular EMS shifts. Additional EMS shifts may limit rest time for paramedics, as several studies reported poor sleep quality due to shift work in this population (for a review, see Sofianopoulos et al., 2012). While there are plausible explanations, the number of EMS shifts was not assessed in the present study and reasons for elevated mental disorder symptoms in HEMS paramedics should be explored further using quantitative and qualitative approaches.
While the prevalence rates of clinically elevated symptoms of post-traumatic stress and major depressive disorder in the present study were higher than previous estimations, it should be noted that both remain at much lower levels compared to other on-the-ground medical and non-medical first responders (e.g., EMS paramedics, police; Carleton et al., 2018). As such, the question remains why HEMS staff are less affected by mental disorder symptoms, despite the unique challenges, stressors, and exposures that come along with working in this field. There are several possible explanations to answer this question, which can be grouped into individual factors and organizational support factors.
Among individual factors are motivations and coping mechanisms. HEMS professionals are required to complete extensive additional training and undergo rigorous selection processes before they are permitted to work in the field. As such, those only especially motivated individuals choose to engage in the additional training and may see the chance to work in HEMS as a privilege (Shalev et al., 2019). In addition, HEMS personnel may possess enhanced coping strategies to manage challenges well. In a recent qualitative study, van Herpen et al. (2024) revealed that HEMS personnel engage in effective coping strategies before, during, and after a dispatch. Before a dispatch, HEMS personnel shared that they have some information to mentally prepare for what lies ahead of them. They will have received some detailed information from other first responders who attended to the scene already. In addition, HEMS personnel were able to separate the quality of their work from the outcome for the patient. Many times, HEMS will be called to missions in which the outcome is almost predetermined. Participants also shared that repeated traumatic scenes become routine, which may help to regulate stress better. During a dispatch, HEMS personnel described that they could create an emotional distance to the scene, as they are able to solely focus on their mission and work. This may entail removing themselves from the scene when their work is done. After a dispatch, HEMS personnel engaged in periods of reflection and structured debrief with others. Family support was also a contributing factor to well-being. Yet, future research is warranted to explore which mechanisms are most effective to enhance short- and long-term coping in HEMS personnel.
From an organizational perspective, several factors were mentioned as well. HEMS personnel remain on a team with the same professionals regularly, fostering trust, team support, and cohesion. Safe conversations about traumatic experiences and the emotional toll of HEMS work can happen in such teams (van Herpen et al., 2024). In this environment, peer support is central to well-being. The effectiveness of peer support may even be magnified in teams with a longer history of working together and enhanced trust. The members might know each other well and can anticipate if someone needs peer support, in some cases without the person sharing their need (van Herpen et al., 2024).
The current study should be interpreted in light of its limitations. The current study did not explore psychological, organizational, or other extraneous factors, which may affect the mental health of HEMS personnel. Future research in this area is warranted to create a deeper understanding of the findings of the present study. While the sample size in the present study is much larger than previous research (e.g., Harenberg et al., 2018; Reid et al., 2022), a portion of eligible participants did not respond to the invitation to complete the survey. Hence, the sample might be biased as only motivated participants may have completed the current study. The cross-sectional nature of data collection further limits its interpretability. Symptoms of mental disorders are fluctuating. Longitudinal studies may shed more light on the prevalence of mental disorder symptoms in HEMS workers over time. Assessing whether HEMS personnel also engaged in EMS or other work would have contributed to the explanation of the presentation of post-traumatic stress and depressive symptoms. Lastly, collecting data whether HEMS personnel engaged in external support to deal with their mental disorder symptoms would have also been of value.
The present study contributes significantly to our understanding of the mental well-being of HEMS personnel in Canada. Previous data (Harenberg et al., 2018) most likely underestimated the emotional burden of HEMS work, due to a smaller sample size and data collection from only the mid-west of Canada, among other reasons. The data from the present study delivers information from a large sample of HEMS participants from six Canadian provinces. Yet, similar to Harenberg et al. (2018), the present study found a relatively low prevalence rate of mental disorder symptoms in HEMS personnel compared to other first responders. While previous research suspected underreporting of symptoms as a possible explanation, new evidence from the present study and recent data from Norway (Reid et al., 2022) may suggest otherwise. These findings may pose novel questions for future research exploring the reasons for the low prevalence rate of mental disorder symptoms in Canadian HEMS.
Future research may wish to apply a biopsychosocial approach. Biologically, it may be worth to explore physiological (e.g., skin conductance, heart rate variability, heart rate) predictors and adaptations to traumatic stress in HEMS work. Associations between physiological markers and PTSD have been well established previously in other populations (Gutner et al., 2010). Some research has explored physiological demands of HEMS work (Carchietti et al., 2011; Petrowski et al., 2023); however, the link between physiological markers and mental well-being in HEMS has yet to be examined. Psychologically, more research is warranted to explore personality factors and coping strategies in HEMS workers. Drawing on the findings by van Herpen et al. (2024), more exploratory studies should assess the relationship between adaptive personality traits, coping mechanisms, and mental disorder symptoms in HEMS personnel. Lastly, research on social perspectives may focus on dynamics within HEMS teams as well as organizational support that may decrease the prevalence of mental disorder symptoms. For example, peer support and team cohesion may be a significant factor in this relationship, with evidence from other fields supporting this hypothesis (e.g., armed forces, Du Preez et al., 2012).
There may also be additional organizational factors. For instance, to our knowledge, there is an absence of research exploring psychological selection criteria of HEMS staff, both for joining the organization and also for the pairing with other professionals. Research in this area may shed more light on the factors that HEMS organizations (in Canada and other countries) consider when making staffing decisions. Based on the recommendations, it is apparent that quantitative, qualitative, and mixed-methods studies may be utilized to answer the questions resulting from the present study. Such research is worthwhile as it may deepen our understanding why initial findings suggest that HEMS workers are emotionally well compared to other first responder and public safety personnel groups with similar traumatic exposure. Such knowledge may assist these groups to further prevent the negative impact of mental disorder symptoms in the workplace.
The authors have no conflicts of interest to declare.
None.
*Department of Human Kinetics, St. Francis Xavier University, 4130 University Ave, Antigonish, NS, Canada;
†Faculty of Graduate Studies and Research, University of Regina, 3737 Wascana Pkwy, Regina, SK, Canada;
‡Department of Emergency Medicine, Saskatchewan Health Authority, 701 Queen St, Saskatoon, SK, Canada;
¶Department of Psychology, University of Regina, 3737 Wascana Pkwy, Regina, SK, Canada.
Albrecht, R., Knapp, J., Theiler, J., Eder, M., Pietsch, U. (2020). Transport of Covid-19 and other highly contagious patients by helicopter and fixed-wing air ambulance: A narrative review and experience of the Swiss air rescue Rega. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine, 28(1), 40. https://doi.org/10.1186/s13049-020-00734-9
Crossref PubMed PMC
American Psychiatric Association. (2022). Diagnostic and statistical manual of mental disorders (5th ed.). Washington, DC: APA Press.
Blevins, C. A., Weathers, F. W., Davis, M. T., Witte, T. K., Domino, J. L. (2015). The posttraumatic stress disorder checklist for DSM-5 (PCL-5): Development and initial psychometric evaluation. Journal of Traumatic Stress, 28(6), 489–498. https://doi.org/10.1002/jts.22059
Crossref PubMed
Carleton, R. N., Afifi, T. O., Turner, S., Tailleu, T., Duranceau, S., LeBeuthillier, D. M., Sareen, J., Ricciardelli, R., MacPhee, R. S., Groll, D., Hozempa, K., Brunet, A., Weekes, J. R., Griffiths, C. T., Abrams, K. J., Jones, N. A., Beshai, S., Cramm, H. A., Dobson, K. S., Hatcher, S., Keane, T. M., Stewart, S. H., Asmundson, G. J. G. (2018). Mental disorder symptoms among public safety personnel in Canada. Canadian Journal of Psychiatry, 63(1), 54–64. https://doi.org/10.1177/0706743717723825
Crossref PMC
Carleton, R. N., Afifi, T. O., Taillieu, T., Turner, S., Krakauer, R., Anderson, G. S., MacPhee, R. S., Ricciardelli, R., Cramm, H. A., Groll, D., McCreary, D. (2019). Exposures to potentially traumatic events among public safety personnel in Canada. Canadian Journal of Behavioural Science, 51, 37–52. https://doi.org/10.1037/cbs0000115
Canadian Institute for Public Safety Research and Treatment (CIPSRT). (2019). Glossary of terms: A shared understanding of the common terms used to describe psychological trauma (version 2.1). https://doi.org/10.37119/10294/9055
Courtney, J. A., Francis, A. J. P., Paxton, S. J. (2013). Caring for the country: Fatigue, sleep and mental health in Australian rural paramedic shift-workers. Journal of Community Health, 38, 178–186. https://doi.org/10.1007/s10900-012-9599-z
Crossref
Carchietti, E., Valent, F., Cecchi, A., Rammer, R. (2011). Influence of stressors on HEMS crewmembers in flight. Air Medical Journal, 30(5), 270–275. https://doi.org/10.1016/j.amj.2011.02.002
Crossref PubMed
Du Preez, J., Sundin, J., Wessely, S., Fear, N. T. (2012). Unit cohesion and mental health in the UK armed forces. Occupational Medicine, 62(1), 47–53. https://doi.org/10.1093/occmed/kqr151
Crossref
Gutner, C. A., Pineles, S. L., Griffin, M. G., Bauer, M. R., Weierich, M. R., Resick, P. A. (2010). Physiological predictors of posttraumatic stress disorder. Journal of Traumatic Stress, 23(6), 775–784. https://doi.org/10.1002/jts.20582
Crossref PubMed PMC
Harenberg, S., McCarron, M., Carleton R. N., O’Malley, T., Ross, T. (2018). Experiences of trauma, depression, anxiety, and stress in Western-Canadian HEMS personnel. Journal of Community Safety Well-Being, 3(2), 18–21. https://doi.org/10.35502/jcswb.62
Crossref
Kessler, R. C., Berglund, P., Demler, O., Jin, R., Merikangas, K. R., Walters, E. E. (2005). Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Archives of General Psychiatry, 62, 593–602. https://doi.org/10.1001/archpsyc.62.6.593
Crossref PubMed
Kroenke, K., Spitzer, R., Williams, J. (2001). The PHQ-9: Validity of a brief depression severity measure. Journal of General Internal Medicine, 16(9), 606–613. https://doi.org/10.1046/j.1525-1497.2001.016009606.x
Crossref PubMed PMC
Lawn, S., Roberts, L., Willis, E., Crouzner, L., Mohammadi, L., Goble, E. (2020). The effects of emergency medical service work on the psychological, physical, and social well-being of ambulance personnel: A systematic review of qualitative research. BMC Psychiatry, 20, 348. https://doi.org/10.1186/s12888-020-02752-4
Crossref PubMed PMC
Lovibond, S. H., Lovibond, P. F. (1995). Manual for the depression anxiety stress scale (2nd ed.). Syndey, Australia: Psychology Foundation.
Petrie, K., Milligan-Saville, J., Gayed, A., Deady, M., Phelps, A., Dell, L., Forbes, D., Bryant, R. A., Calvo, R. A., Glozier, N., Harvey, S. B. (2018). Prevalence of PTSD and common mental disorders amongst ambulance personnel: A systematic review and meta-analysis. Social Psychiatry and Psychiatric Epidemiology, 53, 897–909. https://doi.org/10.1007/s00127-018-1539-5
Crossref PubMed
Petrie, K., Smallwood, N., Pascoe, A., Willis, K. (2022). Mental health symptoms and workplace challenges among Australian paramedics during the COVID-19 pandemic. International Journal of Environmental Research and Public Health, 19(2), 1004. https://doi.org/10.3390/ijerph19021004
Crossref PubMed PMC
Petrowski, K., Malkewitz, C. P., Schöniger, C., Frank, M., Theiler, L. (2023). Stress of emergency physicians during helicopter operations: Impact of patients’ diagnoses, severity of diagnoses, and physicians’ work experience. BMC Emergency Medicine, 23, 20. https://doi.org/10.1186/s12873-023-00786-x
Crossref
Reardon, M., Abrahams, R., Thyer, L., Simpson, P. (2020). Prevalence of burnout in paramedics: A systematic review of prevalence studies. Emergency Medicine Australasia, 32(2), 182–189. https://doi.org/10.1111/1742-6723.13478
Crossref PubMed
Reid, B. O., Næss-Pleym, L. E., Haugland, H., Dale, J., Uleberg, O., Nordstrand, A. E. (2022). Posttraumatic stress responses and psychological well-being in Norwegian medical helicopter personnel. Air Medical Journal, 41(3), 292–297. https://doi.org/10.1016/j.amj.2022.02.006
Crossref PubMed
Shalev, A. Y., Gevonden, M., Ratanatharathorn, A., Laska, E., van der Mei, W. F., Qi, W., Lowe, S., Lai, B. S., Bryant, R. A., Delahanty, D., Matsuoka, Y. J., Olff, M., Schnyder, U., Seedat, S., deRoon-Cassini, T. A., Kessler, R. C., Koenen, K. C., International Consortium to Predict PTSD. (2019). Estimating the risk of PTSD in recent trauma survivors: results of the International Consortium to Predict PTSD (ICPP). World Psychiatry, 18(1), 77–87. https://doi.org/10.1002/wps.20608
Crossref PubMed PMC
Sharma, A., Minh Duc, N. T., Luu Lam Thang, T., Nam, N. H., Ng, S. J., Abbas, K. S., Huy, N. T., Marušić, A., Paul, C. L., Kwok, J., Karbwang, J., de Waure, C., Drummond, F. J., Kizawa, Y., Taal, E., Vermeulen, J., Lee, G. H. M., Gyedu, A., To, K. G., Verra, M. L., Jacqz-Aigrain, E. M., Leclercq, W. K. G., Salminen, S. T., Sherbourne, C. D., Mintzes, B., Lozano, S., Tran, U. S., Matsui, M., Karamouzian, M. (2021). A consensus-based checklist for reporting of survey studies (CROSS). Journal of General Internal Medicine, 36(10), 3179–3187. https://doi.org/10.1007/s11606-021-06737-1
Crossref PubMed PMC
Sofianopoulos, S., Williams, B., Archer, F. (2012). Paramedics and the effects of shift work on sleep: A literature review. Emergency Medicine Journal, 29(2), 152–155. https://doi.org/10.1136/emj.2010.094342
Crossref
van Herpen, M. M., Nieuwe Weme, D., de Leeuw, M. A., Colenbrander, R. J., Olff, M., Te Brake, H. (2024). Wellbeing of helicopter emergency medical services personnel in a challenging work context: A qualitative study. Prehospital Emergency Care, 28(2), 308–317. https://doi.org/10.1080/10903127.2023.2184885
Crossref
Correspondence to: Sebastian Harenberg, 42 West Street, Antigonish, NS, B2G 2W5, Canada. Telephone: 902 867 2157. E-mail: sharenbe@stfx.ca
This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/. For commercial re-use, please contact sales@sgpublishing.ca.
Journal of CSWB, VOLUME 10, NUMBER 2, June 2025