Kyle D. Handley*, R. N. Carleton*, A. A. Deschênes*, J. Devlin*, K. Kamkar*, V. Lee*, R. Mackoff*, C. A. Martin-Doto*, N. Shields*, K. Stockdale*, M. Teale Sapach*
ABSTRACT
This paper traces the emergence of Safeguard programs in Canadian police agencies and explores the research and methods of delivering routine, mandatory mental health check-ups to sworn and civilian personnel in positions with frequent exposure to potentially psychologically traumatic content or situations. A definition for Safeguards is proposed and future directions for police leaders and research are discussed.
Key Words Mental health; police; Safeguard; routine mental health checks.
There is growing recognition that police work presents unique psychological hazards and impacts among sworn and civilian members. Mental health challenges among Canadian police services members, including symptoms of posttraumatic stress disorder (PTSD), continue to be significantly more prevalent than in the general population and are increasingly observed and overrepresented in workplace injury claims. Carleton et al. (2018) initially reported that federal (50.2%) and municipal police (36.7%) across Canada reported higher prevalence of clinically significant mental health symptoms than those reported by the general public. More recently, Carleton et al. (2024) replicated the finding that the majority of Canadian federal police (64.7%) reported clinically significant mental health symptoms. The substantial prevalence of mental health challenges is also evident with increased workplace injury claims. In a review of workplace injury claims, Busque (2022) noted that workplace injury claims for PTSD diagnoses in a Quebec population were 10 times greater for police officers compared to other professions. As a result, many police services are exploring various types of programs and initiatives to support the mental health of their members.
Safeguard programs are one category of proactive mental health strategies that appears increasingly popular in Canada for personnel at heightened risk for PTSD and related disorders. The programs involve routine, mandatory sessions with a psychologist or qualified mental health professional. Despite the widespread interest in developing proactive mental health programs, there does not appear to be a consistent definition or structure for Safeguard programs that has emerged to guide police services, though there have been recent efforts among some police groups to categorize these types of programs (International Association of Chiefs of Police Psychological Services Section, 2023). The following elements appear common among proactive mental health programs using the Safeguard label:
Other Safeguard program elements can inconsistently include psychometric testing, selection, exit contacts pre- and post-placement within designated units, and multi-phase program structures.
A consistent definition for “Safeguard program” is key for effective communication and supporting evaluating program impacts on police mental health. The following is a proposed broad definition for “Safeguard program” in Canada:
A Safeguard program is a formal and coordinated system of routine psychological health checks delivered by a mental health professional to sworn and civilian police members identified by the police service as being uncommonly exposed to potentially psychologically traumatic events or content in the course of their regular duties. Safeguard programs may also be referred to as routine mental health checks, wellness checks, or operational stress management sessions.
The current paper builds upon the proposed definition by providing (1) an overview of the history of Safeguard programs; (2) descriptions of the Safeguard program types used among Canadian police services; (3) the methods for designing and implementing Safeguard programs; and, (4) a series of recommendations for how Safeguard programs can be used and researched in the future.
There are few published, contemporaneous accounts detailing the history of Safeguard programs. The most commonly cited history of Safeguard programs is by Meredith Krause, a former Federal Bureau of Investigation (FBI) Personnel Psychologist. Krause cited a 1998 internal review conducted by the FBI’s industrial organizational psychologists as key evidence for the reliability and validity of the initial Safeguard program; however, the internal research is not available for external peer review (Krause, 2009).
Many Safeguard programs have existed to support police mental health since the 1970s (e.g., the Psychological Services Division of the Calgary Police Service; Celser, 2009); however, widespread implementation of internal mental health services and programs accelerated in the 1990s with the adoption of critical incident stress management teams, and later in the 2000s with police services beginning to offer formalized peer support. A pivotal factor contributing to Safeguard program adoption in Canada was the rapid emergence of provincial legislation that streamlined the process of reporting work-related posttraumatic stress injuries for first responders and other public safety personnel, which facilitated access to care. Many provinces that enacted the presumptive legislation also required impacted organizations to produce proactive plans to mitigate traumatic stress (Ontario Ministry of Labour, 2016), increasing interest in Safeguard programs.
The Ontario Ombudsman’s 2012 In the Line of Duty report was another important catalyst for increased implementation of Canadian Safeguard programs. The same report reviewed the Ontario Provincial Police (OPP)’s approach to operational stress injuries (OSIs; i.e., any mental disorder that develops as a result of exposure to operational stressors within the context of work-related duties as a first responder) and produced a series of recommendations designed to improve the psychological well-being of members. The OPP launched their Safeguard program in 2003, becoming one of the first publicly documented adaptors of Safeguard programming in Canada. The OPP Safeguard program was generally lauded as a success in the Ombudsman’s report based on member feedback; however, the report did not cite any published peer-reviewed empirical evidence in support of the program’s positive impact on OSIs or stigma reduction.
There is limited empirical evidence specifically for Safeguard programs, but there is a wealth of published research that provides theoretical support for using Safeguard programs and for key elements within most Safeguard programs. For example, there is considerable published, peer-reviewed research on the effectiveness of treating various OSIs including, anxiety-, depression-, and trauma-related disorders (e.g., see Courtois et al., 2017 and Kamkar, 2020). Thus, individual psychological interventions delivered by trained, culturally competent registered mental health professionals have the potential to be as effective as those delivered via other programs (e.g., employee and family assistance programs, community mental health services, private services), with Safeguard programs supporting service delivery.
There is also evidence that other occupational stressors (e.g., internal procedures, shift schedules, performance expectations, workplace culture) are just as impactful on police mental health as potentially psychologically traumatic event exposures (Carleton et al., 2020) and can also be mitigated with Safeguard programs. The management of the exposed police officer, by the individual’s police organization, has proven decisive in managing the risk of psychological distress at work (Brown et al., 1996; Burke, 1998; Burke & Mikkelsen, 2006; Deschênes, 2021).
The need for primary, secondary, and tertiary prevention of mental health challenges caused by diverse policing stressors is clear given the available research evidence; however, there are at least three main barriers to help-seeking among police: (1) stigma; (2) worries about confidentiality; and (3) occupation-specific experience with people in the community who present with mental distress (Newell et al., 2022). Police officers also fear being penalized in their career advancement if they ask for help voluntarily (Deschênes et al., 2019). The barriers to accessing mental health resources can be reduced by ensuring confidentiality, providing accessible, uncomplicated resources, and providing police-specific services (Newell et al., 2022).
Most Safeguard programs have mandatory participation that may reduce the stigma associated with accessing support and promote wellness. American officers assigned to complete mandatory counselling have evidenced higher wellness than a similar group of officers who were not (Tanigoshi et al., 2008). Canadian research results have suggested most officers agree mandatory counselling sessions every 2 years would reduce stigma (76%) and normalize help-seeking behaviour (i.e., 87%) (Wlodyka, 2017).
Routine mental health self-monitoring may also support positive mental health. Canadian results with police cadets evidenced daily electronic mental health self-report surveys can reduce symptoms of generalized anxiety disorder, alcohol use disorder, major depressive disorder, panic disorder, and PTSD (Shields et al., 2023). The self-assessments were also associated with fewer symptoms, suggesting frequent self-monitoring may bolster self-awareness and coping (Shields et al., 2023).
Recent results of research with the US military indicated wellness checks were associated with an increased willingness to seek help, higher self-reported resilience, and a decreased likelihood to report stigma-related career concerns (Adler et al., 2024). The authors concluded mandatory wellness checks socialized soldiers to the counselling process, provided tailored information and skills for managing stress, and therein supported mental health (Adler et al., 2024).
Overall, the evidence suggests key elements in many Safeguard programs are effective, despite absent and much-needed direct evaluations of integrated Safeguard programs.
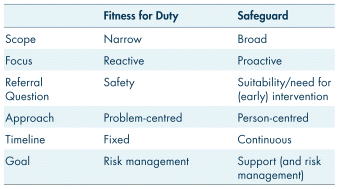
Safeguard programs are often conflated with fitness-for-duty evaluations (FFDEs) and considered opportunities for agencies to engage in direct risk management by providing information about individuals who may be struggling with mental health challenges, which can then be used to inform decisions about work assignments, promotion, transfer, or other personnel decisions. A psychological FFDE “is a formal, specialized examination of an incumbent employee that results from (1) objective evidence that the employee may be unable to safely or effectively perform a defined job and (2) there is a reasonable basis for believing the cause may be attributable to a psychological condition or impairment” (International Association of Chiefs of Police Psychological Services Section, 2018). Accordingly, FFDEs and Safeguard program assessments serve related, but distinct, roles in supporting employee wellness and differ in several important ways (Table I).
TABLE I Fitness-for-duty evaluations vs. Safeguard
Canadian police services would benefit from holistic approaches to adopting and developing Safeguard programs, accounting for key considerations:
The following is a list of questions that can assist services with developing Safeguard program logistics:
The current paper was designed to review the existing literature regarding the history and effectiveness of Safeguard programs as a proactive strategy for promoting psychological health and hardiness in Canadian police officers. A scientific literature review found that Safeguard programs are widely used by Canadian police services, but with no consistent definition, structure, format, or best practices. The lack of a consistent structure complicates evaluations of the effectiveness of Safeguard programs.
The term “Safeguard program” has entered the common parlance in policing environments, being used to describe an internal program that engages a licensed psychologist who offers scheduled mental health check-ups to civilian and sworn members of a police agency. Safeguard implementations appear to vary across services due in part to the lack of a formal definition. As such, we propose the term “Safeguard” be used to describe formal programs that offer routine mental health check-ups to civilian and sworn police members in defined roles and work areas within Canadian police services. Consistently using this definition will provide a foundation to support broader implementations and future research.
There is a dearth of psychological peer-reviewed research related to the effectiveness of Safeguard programs. Regardless, the last 40 years have brought social, political, legislative, and organizational pressures that led many Canadian police services to adopt various forms of Safeguard programs. There is insufficient empirical support specific to Safeguard program effectiveness; nevertheless, there is substantial empirical evidence that psychological interventions are effective for treating various psychological difficulties, including occupational stress injuries such as anxiety-, depression-, and trauma-related disorders (e.g., PTSD). There is also empirical evidence that attending counselling sessions provided as a routine part of employment can help to reduce stigma and increase help-seeking behaviour. The balance of psychological evidence, alongside the emerging literature on wellness checks in other industries, indicates Safeguard programs appear promising for supporting positive mental health outcomes among participants.
The extant literature and pervasive clinical experience evidence that police experience many barriers to psychological help-seeking. Evidence from the USA and Canada indicates Safeguard programs can help to remove stigma related to psychological help-seeking and assist civilian and sworn members seek out support for their psychological wellness.
Safeguard programs must be contextualized as being one component of a service-wide mental health strategy, and not as standalone initiatives. Police services must also avoid conflating Safeguard programs with FFDE, as there are substantial differences in purpose, timing, and implementation. Police services developing a Safeguard program should at least address the aforementioned key considerations and questions to help ensure that the scope and resource allocation are aligned with the organization’s financial realities and expected outcomes.
More work is clearly needed to clarify how to maximize the effectiveness and efficiency of Safeguard programs. Recommendations for future directions can broadly be grouped into the following themes:
Standardization: Improving the consistency of how Safeguard programs are defined, designed, and implemented would facilitate opportunities for outcome research and offer police services a simpler roadmap for building a Safeguard program for their members.
Research: Carrying out formal studies, either internally or in partnership with external research partners, and making the research results broadly available would dramatically improve the understanding of the key components of an effective Safeguard program and the outcomes on police mental health.
Knowledge Translation: Clear communication of the purpose, goals, and impacts of Safeguard programs for both police members and police leaders will assist with buy-in and collaboration. These communications will also help expedite our collective understanding of how Safeguard programs can operate within comprehensive mental health strategies to support the mental health of police.
The above future directions can help clarify the contributions Safeguard programs make within mental health strategies and will help produce best practices for services implementing Safeguard programs.
Overall, early intervention and proactive efforts for addressing mental health challenges are human resources issues that are broadly dependent on a benevolent and supportive management culture, which means each stakeholder has an important role in supporting the mental health of police. Safeguard programs must be driven by a mental health strategy as one piece of larger wellness efforts.
The authors have no conflicts of interest to declare.
*Canadian Association of Chiefs of Police – Psychological Services Committee, Ottawa, ON, Canada
Adler, A. B., Bliese, P. D., Allard, Y. S., Sharp, D. (2024). Wellness checks: Piloting a universal intervention for soldiers. Psychological Services, 21(2), 337–346. https://doi.org/10.1037/ser0000794
Crossref
Brown, J, Coope, C., Kirkcaldy, B. (1996). Occupational stress among senior police officers. British Journal of Psychology, 87, 31–41. https://doi.org/10.1111/j.2044-8295.1996.tb02575.x
Crossref PubMed
Burke, R. J. (1998). Work and non-work stressors and well-being among police officers: The role of coping. Anxiety, Stress, Coping, 11, 345–362. https://doi.org/10.1080/10615809808248319
Crossref
Burke, R. J., Mikkelsen, A. (2006). Burnout among Norwegian police officers: Potential antecedents and consequences. International Journal of Stress Management, 13(1), 64–83. https://doi.org/10.1037/1072-5245.13.1.64
Crossref
Busque, M. A. (2022). Valeurs estimées par le Groupe connaissance et surveillance statistique (GCSS) de la Direction de la recherche de l’IRSST (CNESST; 2015–2019). Montréal, QC: IRSST. Données non publiées.
Carleton, R. N., Afifi, T. O., Turner, S., Taillieu, T., Duranceau, S., LeBouthillier, D. M., Sareen, J., Ricciardelli, R., MacPhee, R. S., Groll, D., Hozempa, K., Brunet, A., Weekes, J. R., Griffiths, C. T., Abrams, K. J., Jones, N. A., Beshai, S., Cramm, H. A., Dobson, K. S., Asmundson, G. J. G. (2018). Mental disorder symptoms among public safety personnel in Canada. Canadian Journal of Psychiatry, 63(1), 54–64. https://doi.org/10.1177/0706743717723825
Crossref PMC
Carleton, R. N., Afifi, T. O., Taillieu, T., Turner, S., Mason, J. E., Ricciardelli, R., McCreary, D. R., Vaughan, A., Anderson, G. S., Krakauer, R., Donnelly, E. A., Camp, R. D. II, Groll, D., Cramm, H. A., MacPhee, R. S., Griffiths, C. T. (2020). Assessing the relative impact of diverse stressors among public safety personnel. International Journal of Environmental Research and Public Health, 17, 1234. https://doi.org/10.3390/ijerph17041234
Crossref PubMed PMC
Carleton, R. N., Jamshidi, L., Nisbet, J., Shields, R. E., Andrews, K. L. (2024). Mental health disorder symptoms among serving Royal Canadian Mounted Police. Police Practice and Research, 25(5), 543–563. https://doi.org/10.1080/15614263.2024.2318209
Crossref
Celser, A. (2009). Psychological services division: Calgary police service. Internal CPS Report (Unpublished).
Courtois, C. A., Sonis, J., Brown, L. S., Cook, J., Fairbank, J. A., Friedman, M., Schulz, P. (2017). Clinical practice guideline for the treatment of posttraumatic stress disorder (PTSD) in adults (pp. 1–119). American Psychological Association.
Deschênes, A.-A. (2021). Organizational levers supporting police officers’ psychological health in the workplace after exposure to a potentially psychologically traumatic event. Advances in Social Sciences Research Journal, 8(8), 301–319. https://doi.org/10.14738/assrj.88.10706
Crossref
Deschênes, A.-A., St-Hilaire, G., Crête, E., Desjardins, C., Emeriau-Farges, C. E. (2019). The potentially traumatic event and the psychological health at work of the police; a perception of a unique impact? American Journal of Applied Psychology, 7(1), 30–35. https://doi.org/10.12691/ajap-7-1-4
Crossref
International Association of Chiefs of Police Psychological Services Section. (2018). Psychological fitness for duty evaluation guidelines. https://www.theiacp.org/working-group/section/psychological-services-section
International Association of Chiefs of Police Psychological Services Section. (2023). Guidelines for wellness visits for law enforcement personnel. https://www.theiacp.org/working-group/section/psychological-services-section
Kamkar, K. (2020, December 10). “Psychology works” fact sheet: Post-traumatic stress disorder. ht tps://cpa.ca/psychology-works-fact-sheet-post-traumatic-stress-disorder/
Krause, M. (2009). History and evolution of the FBI’s undercover safeguard program. Consulting Psychology Journal: Practice and Research, 61(1), 5–13. https://doi.org/10.1037/a0015280
Crossref
Marin, A. (2012). In the line of duty. https://www.ombudsman.on.ca/resources/reports-and-case-summaries/reports-on-investigations/2012/in-the-line-of-duty
Newell, C. J., Ricciardelli, R., Czarnuch, S. M., Martin, K. (2022). Police staff and mental health: Barriers and recommendations for improving help-seeking. Police Practice and Research, 23(1), 111–124. https://doi.org/10.1080/15614263.2021.1979398
Crossref
Ontario Ministry of Labour. (2016). Post-traumatic stress disorder. https://www.labour.gov.on.ca/english/hs/ptsd.php
Shields, R. E., Teckchandani, T. A., Asmundson, G. J. G., Nisbet, J., Krakauer, R., Andrews, K. L., Maguire, K. Q., Jamshidi, L., Afifi, T. O., Lix, L. M., Brunet, A., Sauer-Zavala, S., Krätzig, G. P., Neary, J. P., Sareen, J., Carleton, R. N. (2023). Daily survey participation and positive changes in mental health symptoms scores among Royal Canadian Mounted Police cadets. Frontiers in Psychology, 14, 1145194. https://doi.org/10.3389/fpsyg.2023.1145194
Crossref
Tanigoshi, H., Kontos, A. P., Remley, T. P. (2008). The effectiveness of individual wellness counseling on the wellness of law enforcement officers. Journal of Counseling and Development, 86(1), 63–74. https://doi.org/10.1002/j.1556-6678.2008.tb00627.x
Crossref
Wlodyka, A. (2017). An examination of police stressors and attitudes towards seeking psychological help [Master’s thesis, The University of British Columbia]. Vancouver, BC: cIRcle UBC Theses. https://open.library.ubc.ca/cIRcle/collections/ubctheses/24/items/1.0340912
Correspondence to: Kyle D. Handley, 63 Eric T. Smith Way, Aurora, ON L4G, Canada. Telephone: 905-830-0303 ext. 2490. E-mail: 5926@yrp.ca
This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/. For commercial re-use, please contact sales@sgpublishing.ca.
Journal of CSWB, VOLUME 10, NUMBER 1, March 2025