Alicia M. Hoffman*, Ronald E. Hoffman†, Trevor F. Smith†, Gregory P. Brown†, John P. Hirdes‡
ABSTRACT
The purpose of this study was to identify major characteristics of children and youth with mental health problems who have contact with police officers and to determine which variables lead to the highest probability of police intervention and if there are differences between children and youth compared to adults. Two samples were taken from data obtained from the use of a new police brief mental health screener (interRAI BMHS) in a large southwestern Ontario city between April 2016 and April 2019: 619 cases under age 18 and 4,084 cases over age 18. Univariate and bivariate analysis revealed that all 23 variables on the BMHS were significantly associated with police intervention except for intoxication by drugs or alcohol, squalid home environment, and refusal to take prescribed medication. Variables with the highest odds of police intervention included hallucinations, diminished cognitive skills for daily decision-making, and family or others concerned for potential self-harm. Logistic regression analysis indicated that the variables most predictive of police intervention were hallucinations, lack of insight into their own mental health problems, violent ideation, violence to others, self-injurious attempt in the last 7 days, suicide plan, diminished cognitive skills for daily decision-making, and family or others concerned for self-harm. As to the differences between under and over age 18, adults had higher frequencies of intoxication, hallucinations, delusions, pressured speech, and abnormal thoughts, while under age 18 had slightly higher frequency of socially inappropriate/disruptive behaviour. Risk of harm variables were high in both groups; however, they were clearly higher in the under age 18 group, in particular self-injurious attempt in the last 7 days. The results of this study indicate that there are distinct differences between why police officers intervene with children and youth as opposed to adults which should be reflected in police training and intervention policy.
Key Words Mental illness; screening; child and youth; mental health indicators; early intervention; early identification.
The majority of adults living with mental health issues can trace the onset of their disorders to childhood and adolescence (Patel et al., 2007; Stewart & Hamza, 2017; Stewart & Hirdes, 2015). It is generally accepted that undetected and untreated mental health problems in children and youth can lead to lifelong adverse consequences to the individuals themselves and their families. Recent evidence suggests that the sub-population of children and youth involved in the criminal justice system are particularly vulnerable, many of whom experienced higher rates of exposure to trauma often commencing early in life (Dierkhising et al., 2013; Lyons et al., 1998, 2001; Stewart et al., 2020). Over 60% of children and youth in juvenile detention and correctional facilities have a diagnosable mental health condition (Fazel et al., 2008; Stewart et al., 2015; Teplin et al., 2002), with the most common treatable disorders being depression and attention-deficit hyperactivity disorder (ADHD) in males and posttraumatic stress disorder (PTSD) and even higher levels of depression in females (Beaudry et al., 2021; Fazel et al., 2008). Compared to adults, adolescents in juvenile detention and correctional facilities are at higher risk of self-injury, suicidal ideation, and recent self-harm and are more verbally and physically abusive (Beaudry et al., 2021; Fazel et al., 2008).
It is recognized that due to the unique needs of children and youth with mental health issues who are involved in the correctional system, particular emphasis should be placed on early screening for risk factors (Stewart et al., 2015). Some of the earliest possible junctures for screening and intervention have traditionally been the school system, courts, probation services, and youth detention centres. Yet, undeniably, contact with police officers remains a primary gateway to the criminal justice and mental healthcare systems for children, youth, and adults (Lamb et al., 2002). Police officers have been increasingly called upon to respond to calls for service involving persons with mental disorders as part of their general patrol duties, as members of crisis intervention teams, and as partners in various co-responder models pairing a mental health worker with a police officer (Livingston, 2017; Shore & Lavoie, 2018). However, their involvement is often restricted to instances where the child, youth, or adult is experiencing a mental health crisis or has committed, or likely to commit, a criminal offence. That is, the role of police officers remains predominantly reactive in responding to the crisis or criminal event. There is, however, growing awareness of the potential role police officers could play as an early warning system in proactively identifying and making efforts to connect or re-connect persons, including children and youth, to mental health service providers before they enter the correctional system (Evangelista et al., 2016; van den Brink et al., 2012). To determine if, in fact, it is feasible for police officers to act as part of this early warning system, it is important to review what is known about the frequency and context of police officer involvement, and what are the major clinical characteristics exhibited by the child and youth they interact with.
The research devoted to the subject of police contact with persons with mental health problems is almost entirely focused on adults (Liegghio et al., 2021). For example, it has been well documented that interactions between police officers and persons with mental disorders have been on the rise and continue to rise (Livingston, 2017; Shore & Lavoie, 2018). It is known that about 7–15% of police calls for service involve a person with a mental disorder (Cotton & Coleman, 2008). There is very little empirical evidence on the frequency of calls involving children and youth with mental health problems. However, these calls will likely continue to rise as seen in the adult population. As to the context of police officer interactions, much of what we know is derived from research on adults. About 65% of adults newly admitted to inpatient and community psychiatric services have had some sort of encounter with police over their lifetime (Brink et al., 2011). Also, police interactions with adults often arise in situations where the person poses a threat to themselves or others, is a suspect or victim in criminal activities, or requires transportation to a hospital for psychiatric evaluation (Coleman & Cotton, 2010; Cotton & Coleman, 2008).
Very few studies address the reasons underlying police officer involvement with children and youth with mental health issues. Van der Koep et al. (1997) found that youth using community-based mental health services are nearly three times more likely to be referred to by police officers. Robst et al. (2013) reported that children and youth in group home settings have higher arrest rates than those in inpatient psychiatric settings. Only one study specifically focused on children and youth in contact with police officers based on a community mental health sample of 1,449 children and youth up to 24 years old (Liegghio et al., 2017). About 16% of these service users had police contact related to their mental health. The major reasons for police involvement were similar to those of adults but also include requests for support in the home for a distressed child, as well as concerns about a child’s conduct and behaviour in the community (Liegghio et al., 2017). Specifically, caregivers required help in de-escalating verbal or physical altercations; responding to a child or youth who threatened harm to self or others; managing a child’s behaviour in the community; or transporting the child or youth to hospital due to suicide threats or attempts (Liegghio, 2017; Liegghio & Jaswal, 2015; Liegghio et al., 2017; Liegghio et al., 2020).
Most research on the major clinical characteristics of persons with mental health issues interacting with police is also focused on adults. Typically, research studies have examined the characteristics of adults brought to the emergency department by police officers and compared them to referrals from other sources, such as family, friends, or self-referral (Hoffman, 2013). Adults who are taken to hospital by police officers are most often males in their mid- to late-30s and are more likely to be intoxicated or have substance abuse issues (Hoffman, 2013). They often present with symptoms of psychosis and are considered more severely psychiatrically disturbed than referrals from other sources. Hoffman et al. (2016) reported on the results of the use of a new screener used by police officers, the interRAI Brief Mental Health Screener (BMHS) that captures indicators of major mental health disorders in persons who have police contact. They found that variables significantly associated with psychiatric admission included abnormal thought process, delusions, hallucinations, and little insight into their mental health problems. They also found that there was a higher probability of drug or alcohol use and dangerous and aggressive behaviours toward themselves (Hoffman, 2013; Hoffman et al., 2016). In contrast, although some of the contextual factors have been identified for police officer involvement with children and youth with mental health problems, there are very few data pertaining to clinical characteristics other than generally disruptive behaviour indicative of a distressed child and indicators associated with suicidality.
Currently, there is a gap in knowledge pertaining to the clinical characteristics of children and youth with mental health problems in contact with police officers and the reasons underlying such encounters (Liegghio & Jaswal, 2015; Liegghio et al., 2017, 2020).
The purpose of this study is to use the BMHS to identify the clinical characteristics of children and youth with mental health problems who have contact with police officers and to identify the risk factors that have the highest probability of leading to police intervention. Identifying the signs and symptoms of mental health problems in children and youth would contribute to enhancing police training by providing more detailed information on the indicators of major mental health problems that may lead to early intervention and treatment. It would also assist police officers in determining the most appropriate referrals, whether that is to the hospital or community mental health services.
Data pertaining to the demographic and clinical characteristics of children and youth with mental health disorders having contact with police officers were collected through the use of the interRAI BMHS (Hoffman et al., 2016). The BMHS is a brief mental health screener designed to assist police officers identify key indicators of mental health disorders and document and articulate their grounds for believing that a person has a mental health disorder (Hoffman et al., 2016). A copy of the BMHS can be obtained from interRAI1. It is also used to facilitate improved communication between police officers and mental health service providers as part of an integrated mental health information system (Hirdes et al., 2020; Hoffman et al., 2016, 2021; Pizzingrilli et al., 2015).
The BMHS was developed by interRAI, an international, not-for-profit consortium of researchers committed to improving care for vulnerable persons with complex health needs through evidence-informed clinical practice and policy decision-making (Hirdes et al., 2020). The government of Ontario previously partnered with interRAI to develop and implement the Resident Assessment Instrument for Mental Health (RAI-MH), the assessment system mandated for use on all persons admitted into inpatient psychiatric care in the province (Hirdes et al., 2000/2001). Core items on the BMHS are based primarily on an analysis of RAI-MH data together with input from representatives from healthcare, police services, and patient groups, resulting in the development of the 23-item assessment consisting of three sections: demographical data, a section on clinical indicators of disordered thought, and a section on indicators of risk of harm (Hoffman et al., 2016).
As to the psychometric properties of the BMHS, face validity was achieved through consultation with police officers, mental health professionals, and persons with lived experience who had input into the development of the instrument. Content validity was established through a scoping review of the scientific literature, grey literature, and practical guidelines, and the three sections of the BMHS correspond to police apprehension authorities (indicators of disordered thought, and dangerousness to self or others) as defined in Ontario’s Mental Health Act (Mental Health Act, 1990, s. 17). Also, the development and subsequent approval of the final version was guided by an international clinical and scientific review from the interRAI Network for Mental Health (iNMH) committee and the interRAI Instrument and Systems Development Committee (ISD) (Hoffman et al., 2016). Convergent validity was demonstrated through the association between risk scores on the BMHS and clinical reasons for psychiatric admission. Finally, predictive validity was established through the ability of the items on the BMHS to predict the characteristics of persons transported by the police officer to the hospital and who are ultimately admitted into psychiatric care (Hoffman et al., 2016; Hirdes & Hoffman, 2016; Hirdes et al., 2020).
The BMHS is currently being used by multiple police services in Canada (all western provinces and about half of those in Ontario) and some in the United States. When a police service decides to adopt the BMHS, training is provided for members of the police service’s training branch who then deliver it to their frontline police officers. The training session delivered to frontline police officers consists of explaining the meaning of the items on the screener and how to use the accompanying software. For example, they learn that whenever the BMHS is completed, risk scores are calculated on three scales: danger to self, danger to others, and inability to care for self. The software provides scores on a 10-point scale for each scale and tracks them by date so that the information will be available to police officers who may have subsequent interactions with the same person. Also, if a police officer has difficulty recalling the meaning of particular mental health indicators, such as hallucinations or delusions, by clicking on the item, the definition will appear similar to a tooltip. The police officers are instructed to complete the BMHS on all persons (children, youth, and adults) who they believe may have a mental health disorder, regardless of whether there was evidence of criminal activity. This is particularly important because in the past, police officers typically would not get involved unless there was some form of criminal activity or threat thereof.
As to identifying indicators of mental health disorders, they are told to continue to comply with the appropriate sections of the mental health legislation which are based on three core criteria: danger to self, danger to others, and acting in a disorderly manner. They are informed that the BMHS will help them to better articulate their grounds and in particular, what is meant by acting in a “disorderly manner.” It is explained that the BMHS does not diagnose disorders, rather it helps police officers describe the behaviour they are observing in the language of the health system. That is, the terms used in the screener are consistent with those used in the health system and that by learning and using these terms, it will help them better articulate their grounds for believing someone has a mental health problem. Further, using the same language will help to build a bridge between the criminal justice and health systems and ensure that persons with mental health issues receive help from mental healthcare providers. Finally, it is stressed that the BMHS does not direct their actions but rather is to be used as a decision support tool. The officers must still use their professional judgment regarding the nature of mental health considerations and the need to take the person to a hospital, refer them to a community mental health service provider, or that no action is required.
The setting was a large city in southwestern Ontario which was selected because of its well-established community mental health agencies and three large hospitals. The size of the police service made it possible to obtain enough cases for the study, and members of the police service had been using the BMHS for 2 years and its officers are well acquainted with its purpose and use. Regarding demographics, the population of the city is less than 1 million and is representative of national cultural demographics (about 20% are born internationally) with a variety of ages and socioeconomic backgrounds and a relatively good balance of manufacturing industries, education services, healthcare, technology, and finance.
As part of the licensing agreement with interRAI, police services that use an interRAI instrument submit anonymized information collected through the use of the BMHS to the interRAI Canada database held on secure servers at the University of Waterloo, Ontario. This database is the source of the data used in the current study. A stratified sampling technique was used to identify a sample of 619 unique cases of children and youth, under age 18, and a sample of 4,084 adults, 18 years and over, who had contact with police officers between April 2016 and April 2019.
BMHS assessments were completed electronically on anyone who police officers believed had a mental health issue. The distributions of the variables were calculated for demographic and contextual variables and for those variables related to indicators of disordered thought and indicators of risk of harm. Chi-square analysis was used to determine if there was a statistically significant relationship between individual independent variables on the BMHS and the binary dependent variable; police intervention versus no police intervention and odds ratios (ORs) were computed to estimate the strength of the relationship. Finally, logistic regression was used to investigate the independent effects of individual variables on police intervention and to control for confounding variables (Zhang, 2016). The aim was to examine the joint and independent effects of each of the items on the BMHS to estimate the probability of police intervention.
Police intervention included all cases where the interaction with the individual resulted in the police officer voluntarily escorting the person to the hospital, apprehending them under an existing order, involuntarily apprehending them, or arresting the person. No intervention included cases where the individual was transferred to the emergency medical service (EMS) or the mobile crisis unit, notifying a caseworker or probation officer or referral to a community mental health agency. Police intervention therefore became the dependent variable for the binary logistic regression analysis.
There were two reasons underlying the rationale for the creation of the binary dependent variable police intervention versus no police intervention. First, the term “police intervention” is meant to describe situations where police officers were involved in a more substantive way as opposed to merely referring the person to another agency for follow-up. These interactions would therefore represent a tangible component of a police officer’s job that could be measured and also permit comparisons to be made between the sample of children and youth and the sample of adults. Second, when police are called upon to intervene, their legal authorities require that there is some danger to life or property. Therefore, when police officers are required to intervene, they would be responding to situations that are presumably more serious events. It is important to confirm whether this was the case to ensure that their presence was truly required. That is, do the characteristics exhibited by persons with mental disorders, in fact, require police officers to respond as opposed to other service providers?
Analysis of data from the BMHS assessments from 2016 to 2019 for a medium-sized police service in southwestern Ontario produced two samples: the first included 619 cases between the ages of 6 and 17 and the second included 4,084 cases between the ages of 18 and 96. Police intervention occurred more frequently in under age 18 (68%) versus over age 18 (59%), the majority of whom were between the ages of 13 and 17 (89%), while in the adult sample the majority were under age 44 (68%) with 41% being between ages 25 and 44. Sixty percent of the under age 18 group were females (61%), while the majority in the over age 18 group were males (55%). In the under age 18 sample, two-thirds of the sample (67%) were taken to the hospital (voluntarily or involuntarily) compared to 55% in the over age 18 group with one-third of cases in both groups being referred to a caseworker, probation services, and community mental health agencies. Ten percent of the over age 18 group were identified as homeless compared to 3% of the under age 18 group, and in both groups about one-third of the samples had previous contact with police officers.
With regard to the indicators of disordered thought variables, those in both the under and over age 18 groups exhibited irritability and little to no insight into their mental health problems for more than 50% of the cases. Intoxication by drugs or alcohol was evident twice as often in the over age 18 group (40%) as in the under age 18 group (17%). As to hallucinations and delusions, they were evident in the over age 18 group (51%) versus in the under age 18 group (13%). There was also a higher frequency of the adult sample showing signs of abnormal thought processes (50% vs. 39%) and pressured speech (31% vs. 22%) while the under age 18 group had a slightly higher frequency of socially inappropriate/disruptive behaviour (42% vs. 35%).
As to indicators of risk of harm, self-harm was evident in over half of both samples, particularly for the following variables: considered a self-injurious act in the last 30 days and family or others concern that the person is at risk of self-injury. However, the frequency for both variables was much higher in the under age 18 group at closer to three-quarters of the sample. Similarly, self-injurious attempt in the last 7 days occurred in over 50% of the under age 18 group but only in 33% in the over age 18 group. Suicide plan, violent ideation, and intimidation of others also occurred in over one-third of the under age 18 group but much less in the over age 18 sample.
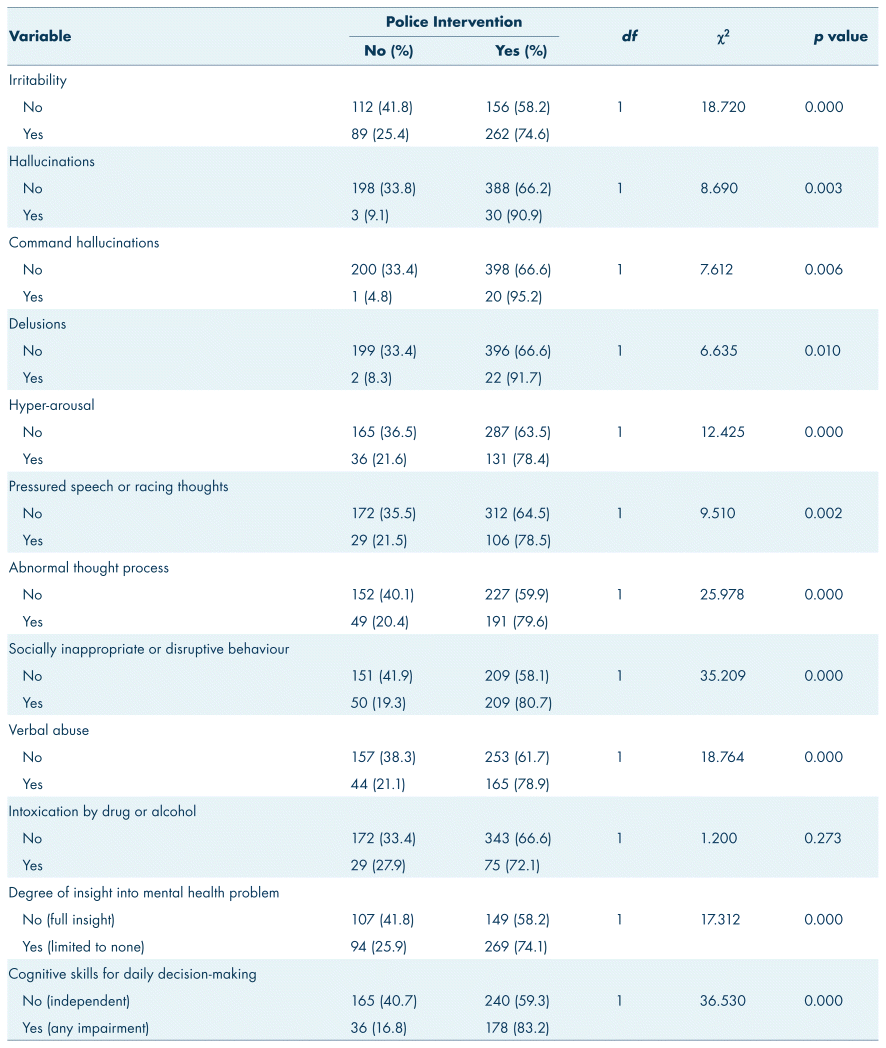
Chi-square analysis revealed that all independent variables in the over age 18 group were significantly associated with police intervention; however, for the under age 18 group the following variables were not significantly associated with police intervention: intoxication (χ2 = 1.2, df = 1, p = 0.273) (Tables I and III), home environment (χ2 = 0.025, df = 1, p = 0.874), and refusal to take medications (χ2 = 1.03, df = 1, p = 0.309) (Tables II and IV).
TABLE I Chi-square analysis of disordered thought variables for under age 18 and police intervention, n = 619
TABLE II Chi-square analysis of risk of harm variables for under age 18 and police intervention, n = 619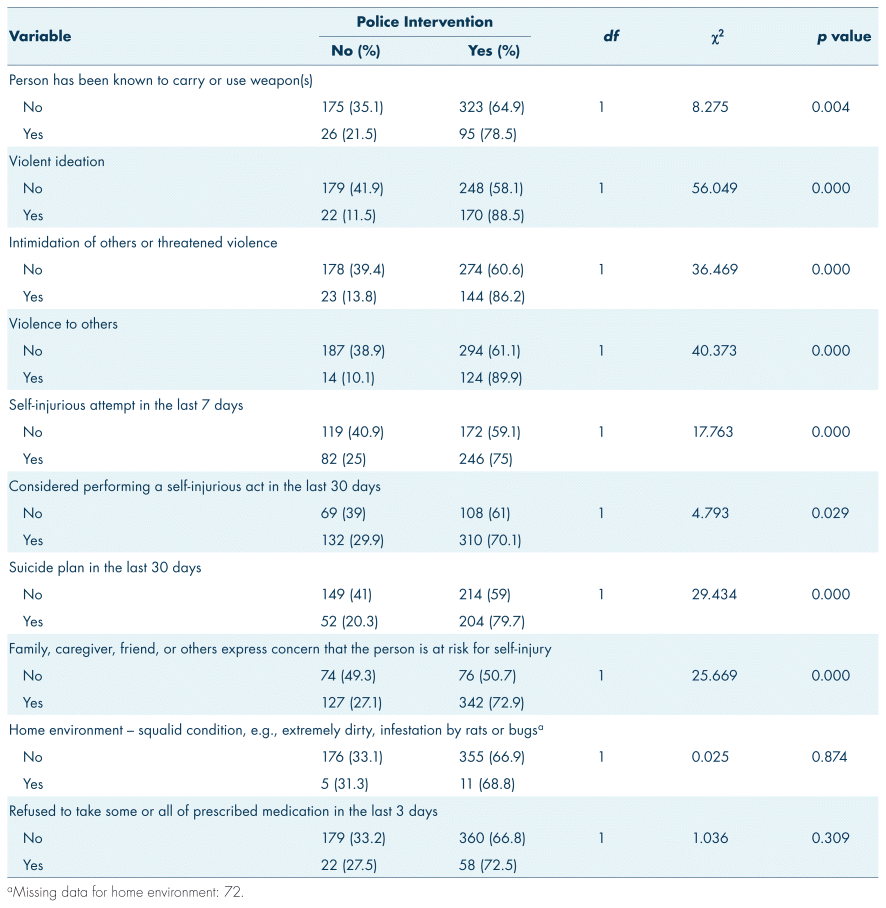
TABLE III Chi-square analysis of disordered thought variables for over age 18 and police intervention, n = 4,083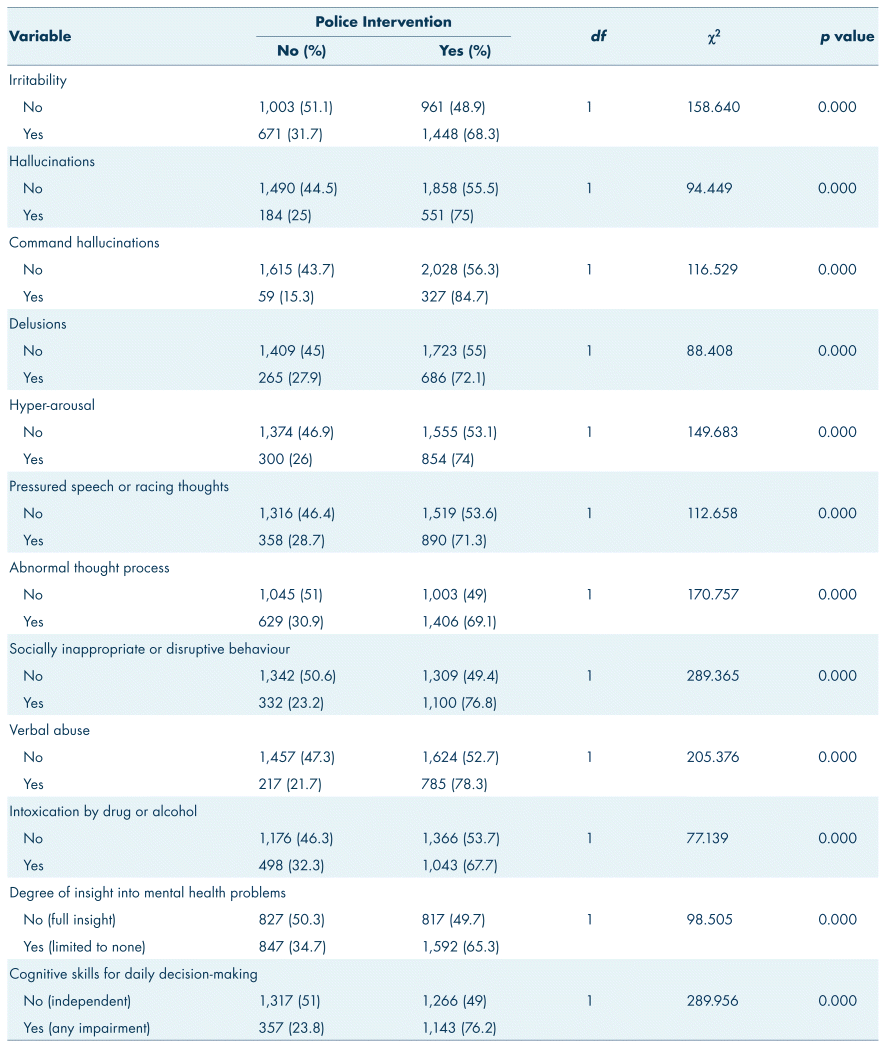
TABLE IV Chi-square analysis of risk of harm variables for over age 18 and police intervention, n = 4,083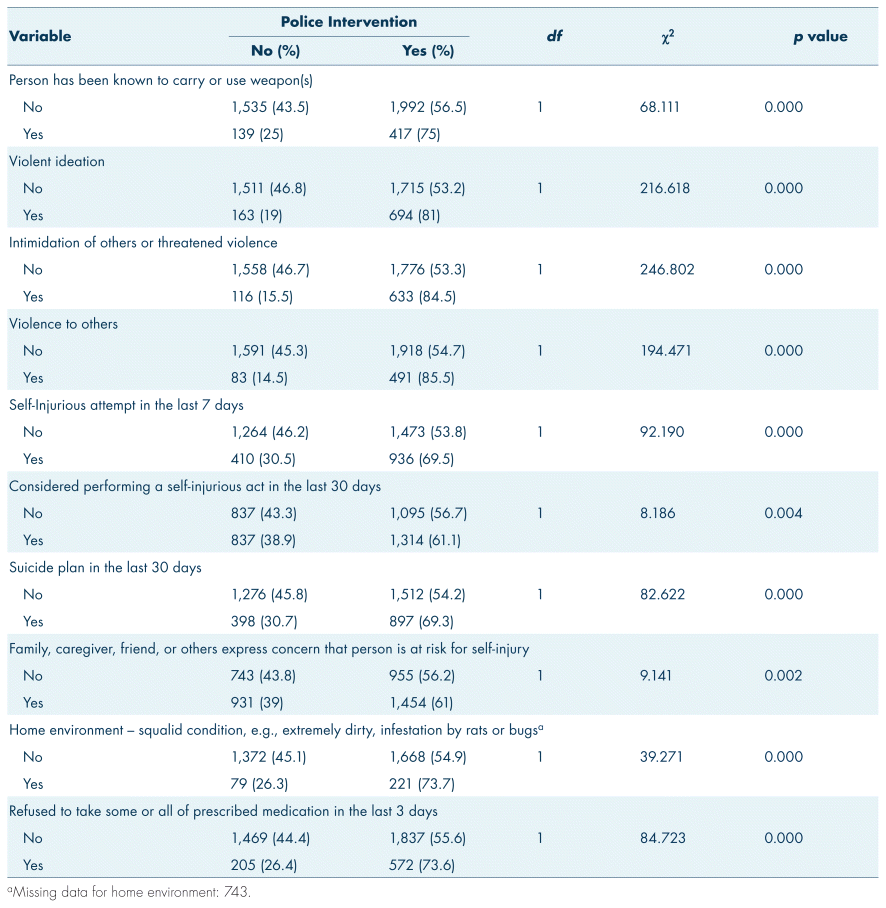
ORs were calculated to measure the strength of the association between the independent variables and police intervention using a convenient cut-off of only those variables where the odds were almost twice as likely for there to be police intervention. For under age 18, the variables with the highest odds of police intervention were hallucinations (OR = 5.93; confidence interval (CI): 0.50–70.01), diminished cognitive skills (OR = 2.0; CI: 1.16–3.44), and family or others concerned for self-harm (OR = 2.09; CI: 1.27–3.44). For over age 18, the variables with the highest odds of police intervention included command hallucinations (OR = 2.36; CI = 1.59–3.50), diminished cognitive skills for daily living (OR = 1.99; CI= 1.66–2.44), self-injurious attempt in the last 7 days (OR = 2.04; CI = 1.67–2.49), suicide plan (OR = 2.13; CI = 1.73–2.61), violence to others (OR = 1.85; CI = 1.22–2.62), and refusal to take medications (OR = 1.78; CI = 1.43–2.21).
Binary logistic regression analysis was used to estimate the probability of police intervention for the over age 18 group, resulting in a model that included hallucinations, command hallucinations, delusions, abnormal thought, socially inappropriate behaviour, intoxication, lack of insight, self-injurious attempt in the last 7 days, suicide plan, known to carry or use weapons, violent ideation, and violence or intimidation of others. The saturated model was applied to the sample of adults producing a c-statistic of 0.73, indicating a good model predictive of police intervention. The same model was applied to the under age 18 group and after removing the variables that were not statistically significant, the resulting model obtained a c-statistic of 0.77.
The model for under age 18 was further refined by adding items shown to have higher odds of police intervention. That is, the variables with the highest odds of police intervention for under age 18 including hallucinations, diminished cognitive skills, and family or others concerned for self-harm were added to the model, and logistic regression analysis was again performed, resulting in a c-statistic of 0.798. A final logistic regression was performed after removing statistically insignificant variables, resulting in the most parsimonious model with a c-statistic of 0.786 (Table V). A summary of the variables that are most related to police intervention comparing under age 18 to over age 18 is presented in Table VI.
TABLE V Logistic regression analysis under age 18 with insignificant variables removed, n = 619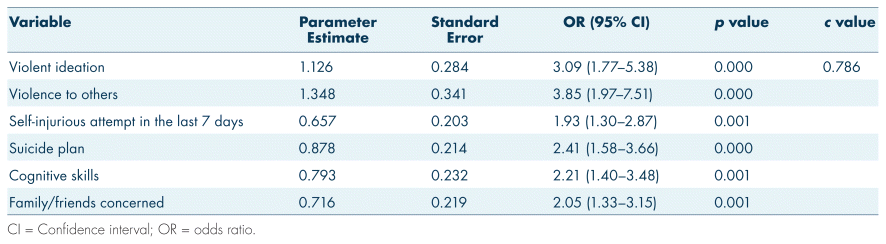
TABLE VI Comparing variables related to police intervention: Under (n = 619) versus over age 18 (n = 4,084)
Through a review of the literature it was determined that little is known about the characteristics of children and youth with mental health problems who have contact with the police. The purpose of this study was to attempt to fill this void by using data generated by the use of the BMHS by the police to identify variables associated with police intervention. Further, the attempt was made to determine how the characteristics of children and youth with mental health problems who have contact with police officers differ from adults with mental health problems. Analysis of data from the BMHS assessments from 2016 to 2019 was used to assist in answering these questions and help fill this gap in the literature.
As mentioned, there is a gap in the literature regarding the clinical characteristics exhibited by children and youth with mental health problems who have contact with police officers. Other than generally disruptive behaviour indicative of a distressed child and behaviours associated with suicidality, very little else was known. However, the current study added significantly to our knowledge regarding additional variables associated with police intervention. Chi-square analysis of the sample for under age 18 revealed that all variables on the BMHS were statistically significant except for intoxication by drugs or alcohol, living in a squalid or extremely dirty home environment (if observed by the officer), and refusal to take prescribed medications with the highest ORs for hallucinations, diminished cognitive skills, and family and others concerned for self-harm. This would appear to be reasonable and consistent with the currently available literature. Adults would have easier access to alcohol due to regulations in Canada. In addition, research shows that youth consume alcohol much less frequently than adults (Harding et al., 2016). Further, children and youth would be most likely supervised when taking prescribed medications. Home environment would probably not be significant as well because parents or caregivers would be responsible for upkeep.
Although suicidality has been identified in the literature as a characteristic of children and youth who have police contact, there is no literature on predictors of police involvement. This study fills a gap in the literature by identifying specific predictor variables. Logistic regression analysis and OR indicated that the variables most predictive included hallucinations, lack of insight into their own mental health problems, violent ideation, violence to others, self-injurious attempt in the last 7 days, suicide plan, diminished cognitive skills for daily decision-making, and family or others concerned for self-harm.
Another aim of this study was to determine if the characteristics of children and youth with mental health problems having contact with police officers differed from those of adults having mental health problems. Results from the univariate analysis of demographic and contextual variables revealed that the sample of children and youth was similar to the sample of adults except for there being a slightly higher frequency of females in the under age 18 group compared to the over age 18 group. In addition, children and youth were more likely to be taken to the hospital by police officers. In terms of indicators of disordered thought, adults had higher frequencies of intoxication, hallucinations, delusions, pressured speech, and abnormal thoughts (hence indicators of though disorder), while under age 18 had slightly higher frequency of socially inappropriate/disruptive behaviours. As to risk of harm variables, indicators of self-harm were high in both groups, but clearly higher in the under age 18 group, in particular self-injurious attempt in the last 7 days.
This analysis identified areas where there were significant differences between children and youth and adults with mental health problems. Through the results of this analysis, it was determined that it was more likely that adult mental health calls for service involve a higher degree of psychiatric disorders such as hallucinations, delusions, command hallucinations, and diminished insight into their mental health problems compared to children and youth. Further, although violent ideation and violence to others were significant predictor variables in both age groups, violence might be considered more pronounced with adults possibly because of the addition of intoxication and weapons. In contrast, children and youth appear to be characterized predominantly by suicidality. Additionally, police encounters with females were more frequent for under age 18, whereas over age 18 males were more frequent. This could be explained by Hagan’s power control theory. Hagan suggested that within patriarchal power relations among family systems, daughters are subject to more supervision than sons. Therefore, parents could be attempting to control their daughters more than their sons (Whitely, 2014).
The results of this study suggest that how police officers respond to children and youth with mental health problems should differ from how they respond to the adult population. Police training needs to be adapted to meet the needs of children and youth. The training police officers receive on responding to children and youth who are experiencing a mental health crisis is minimal at best. It has been reported that police officers receive inadequate training for responding to adults with mental health problems and almost nothing for children and youth. They do not receive sufficient training on the identification of mental health problems, and the information gleaned from this study could be used for such a purpose. For example, training could be provided on how to de-escalate situations where children and youth express violent ideation or violence toward others. Police officers should also pay particular attention to indicators of the child or youth having a suicide plan or having recently attempted to harm themselves and the importance of listening to the concerns of family and friends. The results also demonstrate the importance of family members’ perspectives on mental health needs as a factor influencing the police response to mental health concerns. The BMHS engages family members in two ways: (1) as informants to provide insights into the occurrence of difference mental health indicators; and (2) to report on their own concerns related to the persons’ mental health needs. The former function improves the measurement properties of the BMHS by providing additional sources of information and the latter provides an additional level of sensitivity for identification of self-harm-related risk.
When conducting this study, some limitations were identified. First, there are areas where the BMHS could be analyzed in greater depth, for example, the violence to others variable should receive more study to identify sub-categories. That is, violence to others in children and youth may be simple acting out behaviour or related to suicidality. The literature states that risk factors such as homelessness are associated with substance abuse, sex work, and criminal behaviour, which not surprisingly increase the likelihood of a confrontation with police. It is also reported that a high proportion of homeless youth are experiencing mental health problems. Homeless youth represented too small a proportion of our sample to allow for more detailed investigation. As more data become available from the growing use of the BMHS in North America, it will be possible to undertake future analyses with this small but important population.
The BMHS does not include any items related to school settings. To better understand the setting in which a child or youth makes contact with the police could assist in the training for not only police officers but could help teachers identify early signs of mental health problems. Setting in general may be useful, for example, if a youth is living in a group home; the BMHS can be a source of information to early warning signs and training for group home officials who work closely with children and youth.
In conclusion, the BMHS was found to be useful as a means of identifying characteristics of serious mental disorders in children, youth, and adults. Traditionally, police officers receive basic and in-service training on police officer apprehension authorities under mental health legislation and on major indicators of mental health problems. Almost no training is offered on how mental health disorders are exhibited in children and youth, and the information from the BMHS fills this gap. The ability to identify the characteristics of children and youth who have contact with police officers is significant because it helps to ensure police officers receive appropriate training on how to identify and respond to the signs and symptoms of mental health issues in children and youth. Information from this study could also be used to facilitate early intervention and treatment. In the past, if no criminal activity was involved, police officers would not typically intervene. However, given that the BMHS is completed on anyone who police officers believe may have a mental health disorder, it is possible to identify children and youth who may have been overlooked by parents, school, and agency authorities. Of greater significance, if new referral pathways are created from police officers to local mental health service providers, it would help to facilitate prompt access to mental health services and strengthen the relationship between police services and community mental health service providers.
The authors have no conflicts of interest to declare.
*Department of Sociology and Anthropology, Nipissing University, North Bay, ON, Canada;
†School of Criminal Justice, Nipissing University, North Bay, ON, Canada;
‡School of Public Health and Health Systems, University of Waterloo, Waterloo, ON, Canada.
1https://catalog.interrai.org/BMHS-Police-Assessment-Form-PIY.
Beaudry, G., Yu, R., Långström, N., Fazel, S. (2021). An updated systematic review and meta-regression analysis: Mental disorders among adolescents in juvenile detention and correctional facilities. Journal of the American Academy of Child and Adolescent Psychiatry, 60(1), 46–60. https://doi.org/10.1016/j.jaac.2020.01.015
Crossref PMC
Brink, J., Livingston, J., Desmarais, S., Greaves, C., Maxwell, V., Michalak, E., Parent, R., Verdun-Jones, S., Weaver, C. (2011). A study of how people with mental illness perceive and interact with the police. Mental Health Commission of Canada. https://www.mentalhealthcommission.ca/wp-content/uploads/drupal/Law_How_People_with_Mental_Illness_Perceive_Interact_Police_Study_ENG_1_0_1.pdf
Coleman, T. G., Cotton, D. (2010). Police interactions with persons with a mental illness: Police learning in the environment of contemporary policing. Mental Health Commission of Canada. https://www.mentalhealthcommission.ca/wp-content/uploads/drupal/Law_Police_Interactions_Mental_Illness_Report_ENG_0_1.pdf
Cotton, D., Coleman, T. G. (2008). A study of police academy training and education for new police officers related to working with people with mental illness. Retrieved August 1, 2012, from https://www.mentalhealthcommission.ca/wp-content/uploads/drupal/Law_Police_Academy_Training_Education_Mental_Illness_Study_ENG_0_1.pdf
Dierkhising, C. B., Ko, S. J., Woods-Jaeger, B., Briggs, E. C., Lee, R., Pynoos, R. S. (2013). Trauma histories among justice-involved youth: Findings from the National Child Traumatic Stress Network. European Journal of Psychotraumatology, 4(1), 20274. https://doi.org/10.3402/ejpt.v4i0.20274
Crossref
Evangelista, E., Lee, S., Gallagher, A., Peterson, V., James, J., Warren, N., Henderson, K., Keppich-Arnold, S., Cornelius, L., Deveny, E. (2016). Crisis averted: How consumers experienced a police and clinical early response (PACER) unit responding to a mental health crisis. International Journal of Mental Health Nursing, 25(4), 367–376. https://doi.org/10.1111/inm.12218
Crossref PubMed
Fazel, S., Doll, H., Långström, N. (2008). Mental disorders among adolescents in juvenile detention and correctional facilities: A systematic review and metaregression analysis of 25 surveys. Journal of the American Academy of Child Adolescent Psychiatry, 47(9), 1010–1019. https://doi.org/10.1097/CHI.ObO13e31817eecf3
PubMed
Harding, F. M., Hingson, R. W., Klitzner, M., Mosher, J. F., Brown, J., Vincent, R. M., Dahl, E., Cannon, C. L. (2016). Underage drinking: A review of trends and prevention strategies. American Journal of Preventive Medicine, 51(4), S148–S157. https://doi.org/10.1016/j.amepre.2016.05.020
Crossref PubMed
Hirdes, J. P., Hoffman, R. (2016). Presentation before the International Network for Mental Health (iNMH), Madrid, Spain.
Hirdes, J. P., Marhaba, M., Smith, T. F., Clyburn, L., Mitchell, L., Lemick, R. A., Telegdi, N. C., Pérez, E., Prendergast, P., Rabinowitz, T., Yamauchi, K; Resident Assessment Instrument-Mental Health Group. (2000/2001). Development of the resident assessment instrument - mental health (RAI-MH). Hospital Quarterly, 4(2), 44–51. https://doi.org/10.12927/hcq.2000.16756
Hirdes, J. P., Van Everdingen, C., Ferris, J., Franco-Martin, M., Fries, B. E., Heikkilä, J., Hirdes, A., Hoffman, R., James, M. L., Martin, L., Perlman, C. M., Rabinowitz, T., Stewart, S. L., Van Audenhove, C. (2020). The interRAI suite of mental health assessment instruments: An integrated system for the continuum of care. Frontiers in Psychiatry, 10, 926. https://doi.org/10.3389/fpsyt.2019.00926
Crossref PubMed PMC
Hoffman, R. (2013). Development of the interRAI Brief Mental Health Screener to enhance the ability of police officers to identify persons with serious mental disorder. [Unpublished doctoral dissertation]. University of Waterloo. https://core.ac.uk/reader/144146490
Hoffman, R., Harman, J., Kinsell, H., Brown, G. (2021). Costs and savings associated with the police use of the interRAI brief mental health screener. Frontiers in Psychiatry, 12, 726469. https://doi.org/10.3389/fpsyt.2021.726469
Crossref PubMed PMC
Hoffman, R., Hirdes, J., Brown, G. P., Dubin, J. A., Barbaree, H. (2016). The use of a brief mental health screener to enhance the ability of police officers to identify persons with serious mental disorders. International Journal of Law and Psychiatry, 47, 28–35. https://doi.org/10.1016/j.ijlp.2016.02.031
Crossref PubMed
Lamb, R. H., Weinberger, L. E., DeCuir, W. J. (2002). The police and mental health. Psychiatric Services, 53, 1266–1271. https://doi.org/10.1176/appi.ps.53.10.1266
Crossref PubMed
Liegghio, M. (2017). Our biggest hurdle yet: Caregivers’ encounters with structural stigma in child and youth mental health. Families in Society, 98(4), 300–309. https://doi.org/10.1606/1044-3894.2017.98.35
Crossref
Liegghio, M., Canas, H., Truong, A., Williams, S. (2021). A call for de-policing crisis responses: Distressed children and youth caught between the mental health and police systems. Journal of Community Safety and Well-Being, 6(1), 28–34. https://doi.org/10.35502/jcswb.173
Crossref
Liegghio, M., Jaswal, P. (2015). Police encounters in child and youth mental health: Could stigma informed crisis intervention training (CIT) for parents help? Journal of Social Work Practice, 29(3), 301–319. https://doi.org/10.1080/02650533.2015.1050654
Crossref
Liegghio, M., Truong, A. H., Canas, H., Al-Bader, H. (2020). “I don’t want people to think I’m a criminal”: Calling for more compassionate policing in child and youth mental health. Journal of Community Safety and Well-Being, 5(3), 120–126. https://doi.org/10.35502/jcswb.151
Crossref
Liegghio, M., Van Katwyk, T., Freeman, B., Caragata, L., Sdao-Jarvie, K., Brown, K. C., Sandha, A. (2017). Police encounters among a community sample of children and youth accessing mental health services. Social Work in Mental Health, 15(1), 14–27. https://doi.org/10.1080/15332985.2016.1156043
Crossref
Livingston, J. D. (2017). Contact between police and people with mental disorders: A review of rates. Psychiatric Services, 67(8), 850–857. https://doi.org/10.1176/appi.ps.201500312
Crossref
Lyons, J. S., Libman-Mintzer, L. N., Kisiel, C. L., Shallcross, H. (1998). Understanding the mental health needs of children and adolescents in residential treatment. Professional Psychology: Research and Practice, 29(6), 582–587. https://doi.org/10.1037/0735-7028.29.6.582
Crossref
Lyons, J. S., Royce Baerger, D., Quigley, P., Erlich, J., Griffin, E. (2001). Mental health service needs of juvenile offenders: A comparison of detention, incarceration, and treatment settings. Children’s Services: Social Policy, Research, and Practice, 4(2), 69–85. https://doi.org/10.1207/S15326918CS0402_2
Crossref
Mental Health Act, R.S.O. 1990, c. M.7. Retrieved from https://www.ontario.ca/laws/statute/90m07
Patel, V., Flisher, A. J., Hetrick, S., McGorry, P. (2007). Mental health of young people: A global public-health challenge. The Lancet, 369(9569), 1302–1313. https://doi.org/10.1016/S0140-6736(07)60368-7
Crossref
Pizzingrilli, B., Hoffman, R., Hirdes, D. P. (2015). A protocol to reduce police wait times in the emergency department. Healthcare Management Forum, 28(4), 134–138. https://doi.org/10.1177/0840470415581257
Crossref PubMed
Robst, J., Armstrong, M., Dollard, N., Rohrer, L. (2013). Arrests among youth after out-of-home mental health treatment: Comparisons across community and residential treatment settings. Criminal Behaviour and Mental Health, 23, 162–176. https://doi.org/10.1002/cbm.1871
Crossref PubMed
Shore, K., Lavoie, J. (2018). Exploring mental health-related calls for police service: A Canadian study of police officers as ‘frontline mental health workers’. Policing: A Journal of Policy and Practice, 13(2), 157–171. https://doi.org/10.1093/police/pay017
Crossref
Stewart, S., Baiden, P., den Dunnen, W., Hirdes, J., Perlman, C. M. (2015). Prevalence and correlates of criminal activity in adolescents treated in adult inpatient mental health beds in Ontario, Canada. International Journal of Forensic Mental Health, 14, 33–44. https://doi.org/10.1080/14999013.2015.1014528
Crossref
Stewart, S. L., Hamza, C. A. (2017). The Child and Youth Mental Health Assessment (ChYMH): An examination of the psychometric properties of an integrated assessment developed for clinically referred children and youth. BMC Health Services Research, 17(82), 1–10. https://doi.org/10.1186/s12913-016-1970-9
Crossref
Stewart, S. L., Hirdes, J. P. (2015). Identifying mental health symptoms in children and youth in residential and in-patient care settings. Healthcare Management Forum, 28(4), 150–156. https://doi.org/10.1177/0840470415581240
Crossref PubMed
Stewart, S. L., Thornley, E., Lapshina, N., Erickson, P., Vingilis, E., Hamilton, H., Kolla, N. (2020). Sex differences in youth with mental health problems in inpatient, outpatient and youth justice settings. BMC Psychiatry, 20(1). https://doi.org/10.1186/s12888-019-2413-z
Crossref PubMed PMC
Teplin, L. A., Abram, K. M., McClelland, G. M., Dulcan, M. K., Mericle, A. A. (2002). Psychiatric disorders in youth in juvenile detention. Archives of General Psychiatry, 59(12), 1133–1143. https://doi.org/10.1001/archpsyc.59.12.1133
Crossref PubMed PMC
van den Brink, R. H., Broer, J., Tholen, A. J., Winthorst, W. H., Visser, E., Wiersma, D. (2012). Role of the police in linking individuals experiencing mental health crises with mental health services. BMC Psychiatry, 12(1), 1–7. https://doi.org/10.1186/1471-244X-12-171
Crossref
Whitely, K. M. (2014). Power control theory. Blackwell Publishing Ltd. https://onlinelibrary.wiley.com/doi/abs/10.1002/9781118517383.wbeccj399
Zhang, Z. (2016). Model building strategy for logistic regression: Purposeful selection. Annals of Translational Medicine, 4(6), 111. https://doi.org/10.21037/atm.2016.02.15
Crossref PubMed PMC
Correspondence to: Ronald E. Hoffman, Associate Professor, School of Criminal Justice, Nipissing University, 100 College Drive, Box 5002, North Bay, ON P1B 8L7, Canada. Telephone: 705-474-3450 ext 4565. E-mail: ronhoffman@nipissingu.ca
This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/. For commercial re-use, please contact sales@sgpublishing.ca.
Journal of CSWB, VOLUME 9, NUMBER 2, June 2024