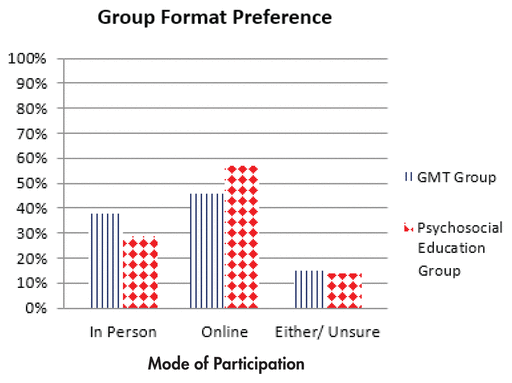
FIGURE 1 Preference for online vs. in-person group sessions
Heather Millman *, Krysta Andrews *†, Sherain Harricharan *†, Sarah Goegan *†, Brahm Sanger *†, Isaac Beech *†, Charlene O’Connor §, Ruth Lanius ‡, Margaret McKinnon *,†§
ABSTRACT
Purpose
This paper explores participants’ perspectives on the acceptability, utility, and perceived therapeutic effects of a virtual group cognitive remediation program, Goal Management Training (GMT) ™ , during the COVID-19 pandemic. The advantages and drawbacks of these groups are considered as part of an online research study protocol exploring cognitive remediation among first responders (police, firefighters, paramedics, emergency dispatchers, corrections and parole officers, and nurses) who have been impacted by trauma.
Methods
We qualitatively examined the results of an anonymous participant feedback survey collected from 20 first responders who took part in the first round of our online therapy groups. A thematic analysis approach was taken to highlight key themes and recommendations.
Results
Survey results indicated that participants found our online protocol effective in terms of group facilitation, the utility of online platforms, and perceived therapeutic effects. Further, some participants preferred participating online versus attending in-person groups.
Conclusion
This early data suggests that providing virtual options for research and treatment among trauma-impacted public safety personnel may increase accessibility and overall participation among this population.
Key Words: Cognitive therapy, group therapy, post-traumatic stress disorder, first responders
The emergence of the current COVID-19 pandemic has resulted in the implementation of emergency response measures at both national and provincial levels in Canada, requiring many Canadians to stay home and reduce their social contact as much as possible. However, public safety personnel (PSP) are required to remain on duty and continue to protect the public throughout the various restrictions. A number of research studies have illustrated how recent pandemics, including COVID-19, affect the mental health of PSP (i.e., first responders—police, fire fighters, paramedics, correctional officers, probation and parole officers, emergency dispatchers, and nurses). Specifically, recent data has revealed significant mental health impacts, including an increased risk of developing post-traumatic stress disorder (PTSD), among health care workers treating ill individuals during pandemics, including patients with COVID-19 in China (Lai et al., 2020; Mo et al., 2020) and patients with MERS in Korea (Lee et al., 2018). In addition, a study exploring perceptions of those treating patients during a potential influenza or smallpox pandemic found that paramedics in the United States reported an increased fear of remaining on duty (Mackler et al., 2007). Collectively, this research provides evidence for increased psychological stress and risk of mental illness experienced by PSP during pandemics.
Among trauma-exposed PSP, recent work has found symptoms of PTSD to be associated with greater risk of cognitive impairment in areas of verbal and visual learning, processing speed, attention, verbal memory, language, and executive functioning; and these cognitive impairments have been linked to poor functional and occupational outcomes (Clouston et al., 2017; Boyd et al., 2019). For PSP, frequent duty-related exposure to trauma can lead to work strain and emotional distress that can compromise an individual’s ability to carry the cognitive load required to comply with the occupational demands of public safety duties (Jones, 2000). In response to these findings, we launched a randomized control trial examining the efficacy of a novel cognitive remediation program, Goal Management Training (GMT)™ (Levine et al., 2000), to aid in improving cognitive deficits among PSP with PTSD. Goal Management Training is a skills-based, cognitive remediation treatment consisting of nine 2-hour sessions that provide individuals with self-monitoring and mindfulness-based strategies, psychosocial education, and other relevant skills in order to reduce the frequency and severity of cognitive difficulties (Levine et al., 2000). Recent studies (Hagen et al., 2020; Cameron et al., 2020; Boyd et al., 2019) have reported improvements in executive functioning and subjective cognition among individuals with certain psychiatric disorders, including PTSD. However, most research trials of GMT have required in-person attendance.
For those already grappling with PTSD and its associated cognitive deficits, the COVID-19 pandemic has made it more difficult to access mental health treatment and support. During widespread lockdowns and social distancing practices, treatment interventions must be available remotely when and where PSP cannot access them in person. To meet this need, we adapted Levine’s GMT program (Levine et al., 2012) into an online protocol that delivers the treatment to PSP remotely. Specifically, our study sought to address a critical gap in the literature by investigating the effectiveness and utility of virtual GMT for trauma-exposed PSP. We hypothesized that, should this virtual protocol be successful in both engaging participants and improving cognitive performance, it will be a critical development in GMT delivery that will increase access to this intervention beyond the context of COVID-19. In the current paper, we detail the adaptations required to offer GMT online and examine the feasibility and patients’ acceptance of this delivery format and related study activities. To evaluate these aspects of our research program, we collected subjective evaluations of our online GMT delivery from our first cohort of participants.
Participants were recruited to the study through social media ads targeting PSP in Ontario and recruitment posters provided to local PSP organizations and support groups. Eligibility was ensured through a screening questionnaire over the phone, and participants were excluded from the study if they lived outside of the province of Ontario, had never worked in an occupation included in the WSIB Operational Policy Manual’s (2018) definition of “first responder,” had a history of neurological disorder, traumatic brain injury, or a medical disorder known to adversely affect cognition, or had an active substance use disorder.
Thirty-three PSP, including police, firefighters, paramedics, correctional and parole officers, emergency dispatchers, and nurses, throughout Ontario participated in our first set of group therapy sessions, using the Zoom for Healthcare video chat platform. Participants were randomized into either the GMT treatment group, or the active control condition, which consisted of psychosocial education. Both conditions completed nine weekly 2-hour group therapy sessions. Groups ranged from seven to ten participants and each was facilitated by a post-doctoral fellow/graduate student researcher and a licensed clinician, including an occupational therapist trained in GMT facilitation.
The primary objective of GMT is to train participants to discontinue ongoing behaviour, define goal hierarchies, and monitor performance (Levine et al., 2011). To achieve this, GMT sessions provided instructional material, interactive tasks, discussion of participants’ real-life challenges, and homework assignments that they completed in personal GMT workbooks. In compliance with GMT protocol, mindfulness meditation exercises were introduced and practiced to help participants train their attentional capacity. A few modifications were required to adapt GMT to online delivery, including changes to tasks requiring participants to work with partners and providing individual copies of some materials that, in traditional in-person GMT delivery, would be re-used by participants, group over group. Participants were mailed copies of the GMT workbook and other materials, including decks of cards and modified task materials, in advance of the group therapy sessions.
The psychosocial education (i.e., active control) group content consisted of a series of modules addressing the neurological and physiological responses to trauma and its effects on lifestyle factors. Specifically, sessions included content on PTSD symptomatology, its impact on areas of cognition (e.g., attention, memory, decision-making), and emotion regulation. Additionally, sessions included group discussions centred on daily challenges involved in living with PTSD, such as social interactions, physical health, nutrition, and sleep hygiene.
Prior to baseline testing, each participant met for an introductory session over Zoom with a member of the research team who acquainted them with the various online testing and meeting platforms used in the study. At baseline, participants completed two semi-structured interviews: the Mini International Neuropsychiatric Interview (MINI) and Clinician Administered PTSD Scale (CAPS-5). At baseline and following the final group session, participants completed cognitive testing involving key domains implicated in PTSD (memory, reasoning, verbal ability, concentration, sustained attention, and processing speed), using the Cambridge Brain Sciences (CBS) and Millisecond Inquisit Web online cognitive testing platforms. In addition, participants also completed the Rey Osterrieth Complex Figure Task (RCFT) and Hooper Verbal Learning Task (HVLT-R). All cognitive testing was carried out while on Zoom with a member of the research team. Following cognitive testing, each participant completed a series of online self-assessments focused on PTSD symptomatology, exposure to traumatic and morally injurious events, executive functioning, and ability to return to work (if applicable). Additional follow-up testing was scheduled for three months and six months post-treatment.
After completing their nine group sessions, participants were asked to use an anonymous group survey to provide feedback about their group experiences and use of the video chat and cognitive testing platforms. The survey asked about three general aspects of participation: 1) perceived effectiveness of group content and therapeutic exercises, 2) utility of online platforms, and 3) preference for virtual compared with in-person group therapy. Once the data was collected, thematic analysis was used to identify similarities and differences in the responses and to highlight significant shared elements (Nowell et al., 2017). These themes were used to explicate key learnings from our first group cohort.
Overall, 20 of the 33 first-round participants responded to the survey, seven of whom participated in the psychosocial education groups and 13 of whom participated in GMT.
Goal Management Training group participants reported that the specialized group activities and homework tasks were most useful in helping them to practice the therapeutic techniques within day-to-day situations. Goal Management Training group members also found that the emphasis on mindfulness strategies helped them to stop and refocus on the task at hand. Interestingly, although specific therapeutic skills were not explicitly taught to members of the Psychosocial Education group, these participants also found that the education provided on “coping techniques” and methods to help control anxiety were helpful in regaining a “sense of agency over one’s brain.” For these participants, learning about the impact of trauma on the brain was especially helpful in understanding their symptoms and cognitive challenges. Members of both groups highlighted a sense of solidarity and interpersonal support with other participants, explaining that participating in groups made them feel “validated” and less “abnormal” or “alone” than they had previously felt. Overall, a majority of participants in both groups felt that the sessions had at least somewhat improved their memory, attention, organization, and concentration (75% of each group, respectively).
We asked participants whether they would prefer to attend GMT or Psychosocial Education therapy sessions in person or online. Those who cited a preference for online group sessions also expressed an appreciation for having a more private, relaxed, and “safe” place in which to participate. As one GMT participant explained, “It was nice being able to participate from the comfort of my own home, in a place I felt safe.” These individuals reported that online sessions reduced or removed the anxiety they attributed to speaking in groups, and helped them to contribute more to group discussions and interact with other participants.
In contrast, those who preferred to attend groups in person found it difficult to interact and connect with other group members online. These individuals hypothesized that in-person groups would provide a greater sense of connection among participants. For instance, one GMT participant explained, “the online group missed out on the benefit of struggling and succeeding as a group. The online [format] took the intimacy of a group setting away.” Given that just under 40% of participants reported a preference for in-person groups, it is important to consider that an online setting may not work best for all PSP, and where feasible, offering both in-person and online options for group participants may optimize the uptake and perceived effectiveness of this therapy. In our online setting, it is notable that despite any drawbacks or difficulties attributed to the online format, no participants dropped out of the study after attending the first group session. In addition, the elimination of transit proved to make online groups more accessible for individuals who maintained their full shift schedule at work, and scheduling make-up sessions for those at work during a group session was easier to arrange. These advantages are represented in the participant feedback survey, wherein many participants from both therapy groups reported a preference for online group sessions (see Figure 1).
|
|
||
|
FIGURE 1 Preference for online vs. in-person group sessions |
||
Anticipating that participants could vary considerably in their technical knowledge and comfort levels navigating through online programs, the research team paid particular attention to the utility of online platforms when designing the protocol. Because assessment tasks required the simultaneous use of a screen and keyboard, participants needed to have access to either a laptop or a desktop computer. Although technical problems did occur, they were rare and were addressed by the research team. When asked how easy they found it to use our video chat and online testing platforms, the majority of participants found all of them to be very easy or somewhat easy (see Figure 2).
|
|
||
|
FIGURE 2 Perceived utility of online platforms |
||
Although our survey did not ask specifically about therapeutic alliance, many participants commented on the group facilitation in the open comment section at the end of the questionnaire. Despite any barriers that video chatting may have presented to relationship building between participants and facilitators, many participants provided positive feedback about the facilitators’ abilities to present materials in a comprehensive and knowledgeable way, and to engage with all participants compassionately and kindly. If a participant was struggling during a session, facilitators were able to discuss the issue with them privately by using the private chat option or Zoom’s “break-out room” feature. This element contributed to participants feeling supported by study staff throughout the sessions.
Participant feedback on our virtual approach to GMT and psychosocial education therapy provides vital insight into the potential for delivering remote group therapy and conducting trauma intervention research online. This finding is especially critical during the COVID-19 pandemic, when unparalleled social restrictions have limited access to mental health care. As health-care providers strive to determine the effectiveness of remote modalities, we highlight the value of understanding participant experiences of online cognitive therapy beyond the context of COVID-19 restrictions. Indeed, we are increasingly recognizing the potential and importance of virtual therapy to reach participants who would not otherwise receive care. While we acknowledge that this approach is not preferred by everyone and limits participation to those with access to reliable internet and a computer at home, we found that our virtual approach did not negatively impact participation rates. In fact, the number of participants increased substantially compared with previous outpatient GMT trials run in person at our locations in the region. Furthermore, attrition rates were significantly lower in our first round than in previous in-person trials. Although some participants voiced a preference for in-person group sessions, they acknowledged that offering the study online was necessary given current pandemic restrictions and actively participated in online sessions.
While our pivot to an online study protocol was a necessary response to the current COVID-19 pandemic, telemedicine and virtual therapy are likely to continue expanding in the post-pandemic world. This predicted expansion is due to telemedicine’s ability to overcome significant barriers to treatment access, such as transportation, time, cost, and the potential stigma of in-person visits. Our transition to online GMT delivery demonstrated that online groups allowed individuals to participate from a broader geographic range than in-person groups. In addition to feeling an increased level of comfort in an at-home setting, a significant number of respondents in our study voiced an overall preference for online participation due to reduced distance and travel time. Thus, we suspect that offering a virtual group GMT and psychosocial education option may be beneficial for trauma-impacted PSP and may facilitate return to work among a broader PSP demographic. Offering such an option removes geographic barriers for participants living in rural and remote areas and may better accommodate those who work rotating shift schedules.
Goal management training, an established and structured cognitive intervention that uses workbooks and other materials, was easily adapted for online delivery with few minor modifications, including providing copies of materials by mail in advance of the sessions. As for the technical challenges involved in an online trial, we found that offering an introductory session during which participants received one-on-one instruction about using the various online platforms was important for those who considered themselves to be less knowledgeable about computers. Also, having research team members available during psychometric testing sessions was pertinent to troubleshoot any technical difficulties.
While the data collected in our participant survey is a helpful first step in understanding the strengths and weaknesses of conducting GMT therapy and collecting psychometric data online, there are several limitations to the data that warrant future investigation. Ideally, we would obtain feedback from a greater proportion of our sample to gather a full understanding of the merits of our virtual therapy and testing. Moreover, because our study required participants to not have been involved in previous in-person GMT trials, they could not compare the groups with an in-person option. It is impossible to know how many PSP could not be recruited for the study because they were not interested in participating online. While those involved in the study were able to access computers to participate, there may be a subset of individuals who could not participate because they do not have access to a computer at home.
Although the team did contact individual PSP organizations to help with recruitment, the majority of our participants responded to our social media ads. It is possible that this led to a greater proportion of participants being comfortable online and having computer access at home, and this could potentially lead to a more positive review of the virtual group environment. Finally, participants provided their subjective opinions about the group’s effectiveness in improving areas of their cognition (e.g., memory, attention, organization, and concentration), but future analysis of the objective data collected during pre- and post-group testing sessions is required to reveal what, if any, cognitive improvements resulted from the two groups.
Our study provides preliminary insight into the benefits and drawbacks of providing cognitive remediation therapy and, more generally, group therapy in an online setting. Despite the loss of face-to-face interaction, participants in our first round of GMT and psychosocial education groups demonstrated that, for many, virtual participation provides a convenient method of attending sessions while maintaining schedules that may otherwise be challenging, such as shift work. Additionally, for those struggling with PTSD and other mental health disorders that may produce anxiety, the ability to participate in therapy while remaining in a familiar and comfortable setting may improve attendance and reduce attrition. An online model also removes physical access barriers that may prevent potential participants from taking part in therapy, such as proximity to urban centres or specialized clinics. For these reasons, while online sessions are not preferrable for all PSP, we propose that offering a virtual alternative for GMT therapy would capture members of the population who would be unable or unwilling to attend in person.
From a research perspective, our ability to adapt our protocol to comply with pandemic restrictions demonstrates that cognitive testing and remediation strategies can be implemented remotely. Specifically, it supports the notion that GMT can be successfully adapted into an online protocol and that virtually administered psychometric testing is reasonable and tolerated by our research population. For PSP, this is particularly salient during times of national emergency, when they must continue to fulfill their role in protecting the public, often at significant personal risk. As recent data has illustrated, global pandemics can increase the risk of developing PTSD among PSP (Lai et al., 2020; Mo et al., 2020; Lee et al., 2018; Mackler et al., 2007). It is thus vital to unveil new avenues for providing accessible therapeutic support during such exceptional times. While future research can further explore the implementation of virtual GMT among a broader patient base (such as first responders outside of Ontario and other populations seeking cognitive remediation therapy) the initial survey results presented here serve to inform not only online approaches to GMT, but also online approaches to clinical care and research in PTSD more broadly.
This work was supported by the Workplace Safety and Insurance Board (Ontario) [grant number MCKI2019 ]. The provision of grant support by WSIB does not in any way infer or imply endorsement of the research findings by the WSIB. M. McKinnon is supported by the Homewood Chair in Mental Health and Trauma at McMaster University. R. Lanius is supported by the Harris-Woodman Chair in Psyche and Soma at Western University. We gratefully acknowledge the in-kind support of the Homewood Research Institute for this project and are very thankful to the participants in the trial.
The authors declare that they have no conflicts of interest.
*
McMaster University, Department of Psychiatry and Behavioural Neuroscience, St. Joseph’s Healthcare, Hamilton, ON, Canada,
†
Homewood Research Institute, Guelph, ON, Canada,
‡
Lawson Health Research Institute, Department of Psychiatry, Western University, Parkwood Institute, London, ON, Canada,
§
Homewood Health Centre, Guelph, ON, Canada.
Boyd, J., O’Connor, C., Protopopescu, A., Jetly, R., Rhind, S., Lanius, R., McKinnon, M. (2019). An open-label feasibility train examining the effectiveness of a cognitive training program, Goal Management Training, in individuals with posttraumatic stress disorder. Chronic Stress, 3, 1–13. https://doi.org/10.1177/2470547019841599
Crossref
Cameron, D. H., McCabe, R. E., Rowa, K., O’Connor, C., McKinnon, M. C. (2020). A pilot study examining the use of Goal Management Training in individuals with obsessive-compulsive disorder. Pilot Feasibility Studies, 6, 151. https://doi.org/10.1186/s40814-020-00684-0
Crossref PubMed PMC
Clouston, S., Guralnik, J., Kotov R., Bromet, E, Luft, B. (2017). Functional limitations among responders to the World Trade Centre attacks 14 years after the disaster: Implications of chronic posttraumatic stress disorder. Journal of Traumatic Stress, 30 (5): 443–452. https://doi.org/10.1002/jts.22219
Crossref PubMed PMC
Jones, S. (2000). Describing the mental health profile of first responders: A systematic review. Journal of the American Psychiatric Nurses Association, 23(3), 200–214. https://doi.org/10.1177/1078390317695266
Crossref
Lai, J., Ma, S., Wang, Y., Cai, Z., Hu, J., Wei, N., Wu, J., Du, H., Chen, T., Li, R., Tan, H., Kang, L., Lao, L., Huang, M., Wang, H., Wang, G., Liu, Z., Shaohua, H. (2020). Factors associated with mental health outcomes among health care workers exposed to Coronavirus disease. JAMA Network Open, 3(3), 1–2. https://doi.org/10.1001/jamanetworkopen.2020.3976
Crossref
Lee, S. M., Kang, W. S., Cho, A. R., Kim, T., Park, J. K. (2018). Psychological impact of the 2015 MERS outbreak on hospital workers and quarantined hemodialysis patients. Comprehensive Psychiatry, 87, 123–127. https://doi.org/10.1016/j.comppsych.2018.10.003
Crossref PubMed PMC
Levine, B., Manly, T., Robertson, I. H. (2012). Trainer’s Manual: Goal Management Training. Toronto: Baycrest Centre for Geriatric Care.
Levine, B., Robertson, I. H. Carter, L., Hong, J., Wilson, B. A., Duncan, J., Stuss, D. T. (2000). Rehabilitation of executive functioning: An experimental-clinical validation of goal management training. Journal of the International Neuropsychological Society, 6 (3), 299–312. https://doi.org/10.1017/S1355617700633052
Crossref PubMed
Levine, B., Schweizer, T. A., O’Connor, C., Turner, G., Gillingham, S., Stuss, D., Manly, T., Robertson, I. H. (2011). Rehabilitation of executive functioning in patients with frontal lobe brain damage with goal management training. Frontiers in Human Neuroscience, 5, 1–9. https://doi.org/10.3389/fnhum.2011.00009
Crossref
Mackler, N., Wilkerson, W., Cinti, S. (2007). Will first-responders show up for work during a pandemic? Lessons from a smallpox vaccination survey of paramedics. Disaster Management Response, 5(2), 45–48. https://doi.org/10.1016/j.dmr.2007.02.002
Crossref PubMed PMC
Mo, Y., Deng, L., Zhang, L., Lang, Q., Liao, C., Wang, N., Qin, M., Huang, H. (2020). Work stress among Chinese nurses to support Wuhan in fighting against COVID-19 epidemic. Journal of Nursing Management, 28(5), 1002–1009. https://doi.org/10.1111/jonm.13014
Crossref PubMed PMC
Nowell, L. S., Norris, J. M., White, D. E., Moules, N. J. Thematic analysis: Striving to meet the trustworthiness criteria. (2017). International Journal of Qualitative Methods, 16, 1–13. https://doi.org/10.1177%2F1609406917733847
Crossref
Workplace Safety and Insurance Board of Ontario (WSIB). (2018). Operational Policy Manual. Retrieved from https://www.wsib.ca/en/operational-policy-manual/posttraumatic-stress-disorder-first-responders-and-other-designated.
This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/. For commercial re-use, please contact sales@sgpublishing.ca.
Journal of CSWB, VOLUME 7, NUMBER 1, March 2022